Page 20 - Read Online
P. 20
Castán et al. Radiology of hepatocarcinoma in non-cirrhotic patients
A B C
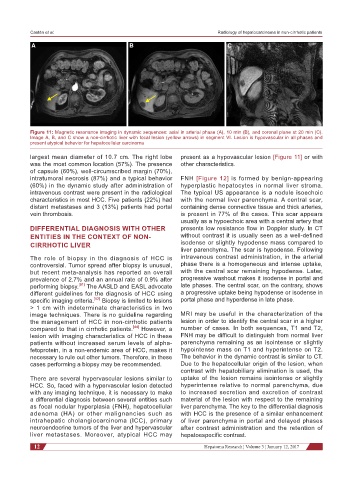
Figure 11: Magnetic resonance imaging in dynamic sequences: axial in arterial phase (A), 10 min (B), and coronal plane at 20 min (C).
Image A, B, and C show a non-cirrhotic liver with focal lesion (yellow arrows) in segment VI. Lesion is hypovascular in all phases and
present atypical behavior for hepatocellular carcinoma
largest mean diameter of 10.7 cm. The right lobe present as a hypovascular lesion [Figure 11] or with
was the most common location (57%). The presence other characteristics.
of capsule (60%), well-circumscribed margin (70%),
intratumoral necrosis (87%) and a typical behavior FNH [Figure 12] is formed by benign-appearing
(60%) in the dynamic study after administration of hyperplastic hepatocytes in normal liver stroma.
intravenous contrast were present in the radiological The typical US appearance is a nodule isoechoic
characteristics in most HCC. Five patients (22%) had with the normal liver parenchyma. A central scar,
distant metastases and 3 (13%) patients had portal containing dense connective tissue and thick arteries,
vein thrombosis. is present in 77% of the cases. This scar appears
usually as a hypoechoic area with a central artery that
DIFFERENTIAL DIAGNOSIS WITH OTHER presents low resistance flow in Doppler study. In CT
ENTITIES IN THE CONTEXT OF NON- without contrast it is usually seen as a well-defined
CIRRHOTIC LIVER isodense or slightly hypodense mass compared to
liver parenchyma. The scar is hypodense. Following
The role of biopsy in the diagnosis of HCC is intravenous contrast administration, in the arterial
controversial. Tumor spread after biopsy is unusual, phase there is a homogeneous and intense uptake,
but recent meta-analysis has reported an overall with the central scar remaining hypodense. Later,
prevalence of 2.7% and an annual rate of 0.9% after progressive washout makes it isodense in portal and
performing biopsy. [51] The AASLD and EASL advocate late phases. The central scar, on the contrary, shows
different guidelines for the diagnosis of HCC using a progressive uptake being hypodense or isodense in
specific imaging criteria. [52] Biopsy is limited to lesions portal phase and hyperdense in late phase.
> 1 cm with indeterminate characteristics in two
image techniques. There is no guideline regarding MRI may be useful in the characterization of the
the management of HCC in non-cirrhotic patients lesion in order to identify the central scar in a higher
compared to that in cirrhotic patients. [44] However, a number of cases. In both sequences, T1 and T2,
lesion with imaging characteristics of HCC in these FNH may be difficult to distinguish from normal liver
patients without increased serum levels of alpha- parenchyma remaining as an isointense or slightly
fetoprotein, in a non-endemic area of HCC, makes it hypointense mass on T1 and hyperintense on T2.
necessary to rule out other tumors. Therefore, in these The behavior in the dynamic contrast is similar to CT.
cases performing a biopsy may be recommended. Due to the hepatocellular origin of the lesion, when
contrast with hepatobiliary elimination is used, the
There are several hypervascular lesions similar to uptake of the lesion remains isointense or slightly
HCC. So, faced with a hypervascular lesion detected hyperintense relative to normal parenchyma, due
with any imaging technique, it is necessary to make to increased secretion and excretion of contrast
a differential diagnosis between several entities such material of the lesion with respect to the remaining
as focal nodular hyperplasia (FNH), hepatocellular liver parenchyma. The key to the differential diagnosis
adenoma (HA) or other malignancies such as with HCC is the presence of a similar enhancement
intrahepatic cholangiocarcinoma (ICC), primary of liver parenchyma in portal and delayed phases
neuroendocrine tumors of the liver and hypervascular after contrast administration and the retention of
liver metastases. Moreover, atypical HCC may hepatoespecific contrast.
12 Hepatoma Research ¦ Volume 3 ¦ January 12, 2017