Page 188 - Read Online
P. 188
beta2-microglobulin as well as serum protein
electrophoresis and HIV serology were realized and
all these results were normal. Chest X-ray, computed
tomography (CT) scan of the thorax, abdomen, and
pelvis and MRI on the whole neuraxes showed no
other sites of lymphoma and the final diagnosis was
a primary diffuse BCL-2 vertebral body. Adjuvant
LMB-89 chemotherapy treatment was started.
Clinically, the patient was enrolled under an intensive care
and rehabilitation program. Her condition remarkably
a b c
improved and complete recovery was reached within
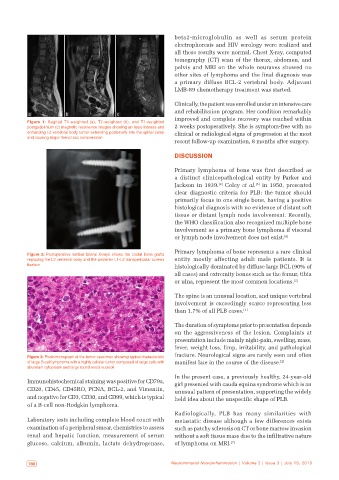
Figure 1: Sagittal T1‑weighted (a), T2‑weighted (b), and T1‑weighted
postgadolinium (c) magnetic resonance images showing an hypo intense and 2 weeks postoperatively. She is symptom-free with no
enhancing L2 vertebral body tumor extending posteriorly into the spinal canal clinical or radiological signs of progression at the most
and causing major thecal sac compression
recent follow-up examination, 8 months after surgery.
DISCUSSION
Primary lymphoma of bone was first described as
a distinct clinicopathological entity by Parker and
Jackson in 1939. Coley et al. in 1950, presented
[5]
[2]
clear diagnostic criteria for PLB: the tumor should
primarily focus in one single bone, having a positive
histological diagnosis with no evidence of distant soft
tissue or distant lymph node involvement. Recently,
the WHO classification also recognized multiple bone
involvement as a primary bone lymphoma if visceral
or lymph node involvement does not exist. [6]
Primary lymphoma of bone represents a rare clinical
Figure 2: Postoperative lumbar lateral X‑rays shows the costal bone grafts
replacing the L2 vertebral body and the posterior L1‑L3 transpedicular screws entity mostly affecting adult male patients. It is
fixation histologically dominated by diffuse large BCL (90% of
all cases) and extremity bones such as the femur, tibia
or ulna, represent the most common locations. [2]
The spine is an unusual location, and unique vertebral
involvement is exceedingly scarce representing less
than 1.7% of all PLB cases. [3]
The duration of symptoms prior to presentation depends
on the aggressiveness of the lesion. Complaints at
presentation include mainly night-pain, swelling, mass,
fever, weight loss, limp, irritability, and pathological
fracture. Neurological signs are rarely seen and often
Figure 3: Photomicrograph of the tumor specimen showing typical characteristic
of large B‑cell lymphoma with a highly cellular tumor composed of large cells with manifest late in the course of the disease. [2]
abundant cytoplasm and large round ovoid nucleoli
In the present case, a previously healthy, 24-year-old
Immunohistochemical staining was positive for CD79a, girl presented with cauda equina syndrome which is an
CD20, CD45, CD45RO, PCNA, BCL-2, and Vimentin, unusual pattern of presentation, supporting the widely
and negative for CD3, CD30, and CD99, which is typical held idea about the unspecific shape of PLB.
of a B-cell non-Hodgkin lymphoma.
Radiologically, PLB has many similarities with
Laboratory tests including complete blood count with metastatic disease although a few differences exists
examination of a peripheral smear, chemistries to assess such as patchy sclerosis on CT or bone marrow invasion
renal and hepatic function, measurement of serum without a soft tissue mass due to the infiltrative nature
glucose, calcium, albumin, lactate dehydrogenase, of lymphoma on MRI. [7]
180 Neuroimmunol Neuroinflammation | Volume 2 | Issue 3 | July 15, 2015 Neuroimmunol Neuroinflammation | Volume 2 | Issue 3 | July 15, 2015 181