Page 482 - Read Online
P. 482
Page 4 of 15 Smer et al. Mini-invasive Surg 2020;4:52 I http://dx.doi.org/10.20517/2574-1225.2020.36
Table 1. Etiology and mechanism of mitral regurgitation
Etiology of mitral regurgitation Mechanism of mitral regurgitation
Atrial fibrillation Annular dilation, leaflet mal-coaptation
Acute ischemia Papillary muscle dysfunction or rupture
Congenital or genetic disorders; Marfan syndrome, Ehlers-Danlos Leaflet prolapse, cleft or rudimentary leaflets
syndrome, Down syndrome
Endocarditis; infective and marantic Leaflet perforation, mal-coaptation, chordal rupture
Drugs; fenfluramine and dexfenfluramine Leaflets, chordae
Functional/secondary; dilated cardiomyopathy Left ventricular remolding, papillary muscle displacement
leading to leaflet tethering and annulus dilation
Hypertrophic obstructive cardiomyopathy Systolic anterior motion of anterior mitral valve leaflet
Myxomatous degeneration (primary)
(1) Barlow’s disease Leaflets prolapse
(2) Fibroelastic deficiency Rupture chordae
Mitral annular calcifications Annulus, leaflets
Rheumatic heart disease Leaflets, chordae
Radiation Leaflets, chordae
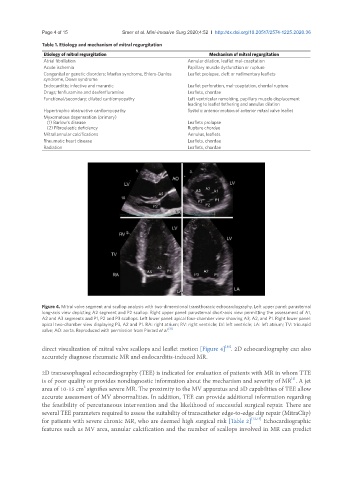
Figure 4. Mitral valve segment and scallop analysis with two-dimensional transthoracic echocardiography. Left upper panel: parasternal
long-axis view depicting A2 segment and P2 scallop. Right upper panel: parasternal short-axis view permitting the assessment of A1,
A2 and A3 segments and P1, P2 and P3 scallops. Left lower panel: apical four-chamber view showing A3, A2, and P1. Right lower panel:
apical two-chamber view displaying P3, A2 and P1. RA: right atrium; RV: right ventricle; LV: left ventricle; LA: left atrium; TV: tricuspid
[11]
valve; AO: aorta. Reproduced with permission from Pierard et al.
direct visualization of mitral valve scallops and leaflet motion [Figure 4] . 2D echocardiography can also
[11]
accurately diagnose rheumatic MR and endocarditis-induced MR.
2D transesophageal echocardiography (TEE) is indicated for evaluation of patients with MR in whom TTE
is of poor quality or provides nondiagnostic information about the mechanism and severity of MR . A jet
[2]
2
area of 10-15 cm signifies severe MR. The proximity to the MV apparatus and 3D capabilities of TEE allow
accurate assessment of MV abnormalities. In addition, TEE can provide additional information regarding
the feasibility of percutaneous intervention and the likelihood of successful surgical repair. There are
several TEE parameters required to assess the suitability of transcatheter edge-to-edge clip repair (MitraClip)
for patients with severe chronic MR, who are deemed high surgical risk [Table 2] [12,13] Echocardiographic
features such as MV area, annular calcification and the number of scallops involved in MR can predict