Page 204 - Read Online
P. 204
Salas et al. J Cancer Metastasis Treat 2018;4:15 I http://dx.doi.org/10.20517/2394-4722.2017.66 Page 9 of 13
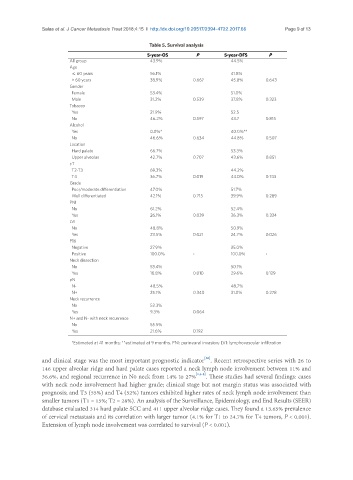
Table 5. Survival analysis
5-year-OS P 5-year-DFS P
All group 43.9% 44.5%
Age
≤ 60 years 56.1% 41.8%
> 60 years 38.9% 0.667 45.8% 0.643
Gender
Female 53.4% 51.0%
Male 31.2% 0.539 37.8% 0.323
Tobacco
Yes 21.9% 52.5
No 46.2% 0.597 43.7 0.815
Alcohol
Yes 0.0%* 40.0%**
No 46.6% 0.634 44.8% 0.507
Location
Hard palate 66.7% 53.3%
Upper alveolus 42.7% 0.707 43.6% 0.851
cT
T2-T3 69.3% 44.2%
T4 36.7% 0.019 44.0% 0.743
Grade
Poor/moderate differentiation 47.0% 51.7%
Well differentiated 42.1% 0.715 39.9% 0.289
PNI
No 61.2% 52.4%
Yes 26.1% 0.039 36.3% 0.334
LVI
No 48.8% 50.9%
Yes 23.5% 0.021 24.7% 0.026
P16
Negative 27.9% 35.0%
Positive 100.0% - 100.0% -
Neck dissection
No 53.4% 50.1%
Yes 18.8% 0.010 29.6% 0.129
pN
N- 48.5% 48.7%
N+ 25.1% 0.340 31.0% 0.278
Neck recurrence
No 52.3%
Yes 9.3% 0.064
N+ and N- with neck recurrence
No 55.5%
Yes 21.6% 0.192
*Estimated at 41 months; **estimated at 9 months. PNI: perineural invasion; LVI: lymphovascular infiltration
[30]
and clinical stage was the most important prognostic indicator . Recent retrospective series with 26 to
146 upper alveolar ridge and hard palate cases reported a neck lymph node involvement between 11% and
36.6%, and regional recurrence in N0 neck from 14% to 27% [1,5-8] . These studies had several findings: cases
with neck node involvement had higher grade; clinical stage but not margin status was associated with
prognosis; and T3 (55%) and T4 (52%) tumors exhibited higher rates of neck lymph node involvement than
smaller tumors (T1 = 15%; T2 = 28%). An analysis of the Surveillance, Epidemiology, and End Results (SEER)
database evaluated 314 hard palate SCC and 411 upper alveolar ridge cases. They found a 13.65% prevalence
of cervical metastasis and its correlation with larger tumor (4.1% for T1 to 24.7% for T4 tumors, P < 0.001).
Extension of lymph node involvement was correlated to survival (P < 0.001).