Page 200 - Read Online
P. 200
Salas et al. J Cancer Metastasis Treat 2018;4:15 I http://dx.doi.org/10.20517/2394-4722.2017.66 Page 5 of 13
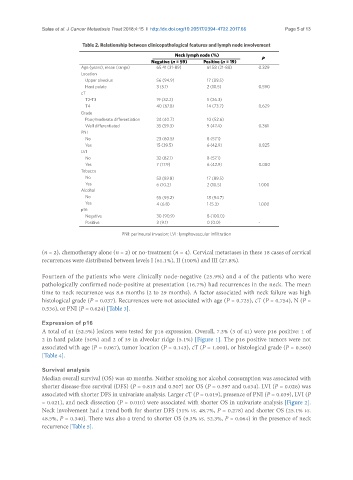
Table 2. Relationship between clinicopathological features and lymph node involvement
Neck lymph node (%) P
Negative (n = 59) Positive (n = 19)
Age (years), mean (range) 65.41 (31-89) 61.58 (21-88) 0.329
Location
Upper alveolus 56 (94.9) 17 (89.5)
Hard palate 3 (5.1) 2 (10.5) 0.590
cT
T2-T3 19 (32.2) 5 (26.3)
T4 40 (67.8) 14 (73.7) 0.629
Grade
Poor/moderate differentiation 24 (40.7) 10 (52.6)
Well differentiated 35 (59.3) 9 (47.4) 0.361
PNI
No 23 (60.5) 8 (57.1)
Yes 15 (39.5) 6 (42.9) 0.825
LVI
No 32 (82.1) 8 (57.1)
Yes 7 (17.9) 6 (42.9) 0.080
Tobacco
No 53 (89.8) 17 (89.5)
Yes 6 (10.2) 2 (10.5) 1.000
Alcohol
No 55 (93.2) 18 (94.7)
Yes 4 (6.8) 1 (5.3) 1.000
p16
Negative 30 (90.9) 8 (100.0)
Positive 3 (9.1) 0 (0.0) -
PNI: perineural invasion; LVI: lymphovascular infiltration
(n = 2), chemotherapy alone (n = 2) or no-treatment (n = 4). Cervical metastases in these 18 cases of cervical
recurrences were distributed between levels I (61.1%), II (100%) and III (27.8%).
Fourteen of the patients who were clinically node-negative (25.9%) and 4 of the patients who were
pathologically confirmed node-positive at presentation (16.7%) had recurrences in the neck. The mean
time to neck recurrence was 8.6 months (2 to 29 months). A factor associated with neck failure was high
histological grade (P = 0.037). Recurrences were not associated with age (P = 0.725), cT (P = 0.754), N (P =
0.536), or PNI (P = 0.624) [Table 3].
Expression of p16
A total of 41 (52.5%) lesions were tested for p16 expression. Overall, 7.3% (3 of 41) were p16 positive: 1 of
2 in hard palate (50%) and 2 of 39 in alveolar ridge (5.1%) [Figure 1]. The p16 positive tumors were not
associated with age (P = 0.067), tumor location (P = 0.143), cT (P = 1.000), or histological grade (P = 0.560)
[Table 4].
Survival analysis
Median overall survival (OS) was 40 months. Neither smoking nor alcohol consumption was associated with
shorter disease-free survival (DFS) (P = 0.815 and 0.507) nor OS (P = 0.597 and 0.634). LVI (P = 0.026) was
associated with shorter DFS in univariate analysis. Larger cT (P = 0.019), presence of PNI (P = 0.039), LVI (P
= 0.021), and neck dissection (P = 0.010) were associated with shorter OS in univariate analysis [Figure 2].
Neck involvement had a trend both for shorter DFS (31% vs. 48.7%, P = 0.278) and shorter OS (25.1% vs.
48.5%, P = 0.340). There was also a trend to shorter OS (9.3% vs. 52.3%, P = 0.064) in the presence of neck
recurrence [Table 5].