Page 202 - Read Online
P. 202
Salas et al. J Cancer Metastasis Treat 2018;4:15 I http://dx.doi.org/10.20517/2394-4722.2017.66 Page 7 of 13
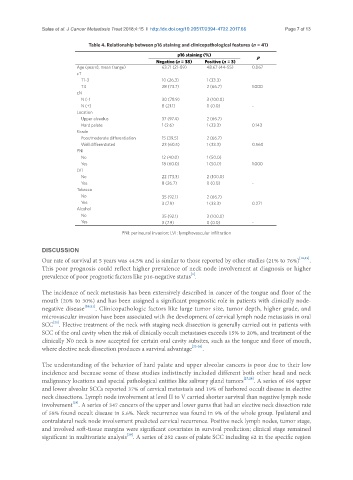
Table 4. Relationship between p16 staining and clinicopathological features (n = 41)
p16 staining (%)
Negative (n = 38) Positive (n = 3) P
Age (years), mean (range) 63.71 (21-89) 48.67 (44-55) 0.067
cT
T1-3 10 (26.3) 1 (33.3)
T4 28 (73.7) 2 (66.7) 1.000
cN
N (-) 30 (78.9) 3 (100.0)
N (+) 8 (21.1) 0 (0.0) -
Location
Upper alveolus 37 (97.4) 2 (66.7)
Hard palate 1 (2.6) 1 (33.3) 0.143
Grade
Poor/moderate differentiation 15 (39.5) 2 (66.7)
Well differentiated 23 (60.5) 1 (33.3) 0.560
PNI
No 12 (40.0) 1 (50.0)
Yes 18 (60.0) 1 (50.0) 1.000
LVI
No 22 (73.3) 2 (100.0)
Yes 8 (26.7) 0 (0.0) -
Tobacco
No 35 (92.1) 2 (66.7)
Yes 3 (7.9) 1 (33.3) 0.271
Alcohol
No 35 (92.1) 3 (100.0)
Yes 3 (7.9) 0 (0.0) -
PNI: perineural invasion; LVI: lymphovascular infiltration
DISCUSSION
Our rate of survival at 5 years was 44.5% and is similar to those reported by other studies (21% to 76%) [18,19] .
This poor prognosis could reflect higher prevalence of neck node involvement at diagnosis or higher
[1]
prevalence of poor prognotic factors like p16-negative status .
The incidence of neck metastasis has been extensively described in cancer of the tongue and floor of the
mouth (20% to 30%) and has been assigned a significant prognostic role in patients with clinically node-
negative disease [20,21] . Clinicopathologic factors like large tumor size, tumor depth, higher grade, and
microvascular invasion have been associated with the development of cervical lymph node metastasis in oral
[21]
SCC . Elective treatment of the neck with staging neck dissection is generally carried out in patients with
SCC of the oral cavity when the risk of clinically occult metastases exceeds 15% to 20%, and treatment of the
clinically N0 neck is now accepted for certain oral cavity subsites, such as the tongue and floor of mouth,
where elective neck dissection produces a survival advantage [22-26] .
The understanding of the behavior of hard palate and upper alveolar cancers is poor due to their low
incidence and because some of these studies indistinctly included different both other head and neck
malignancy locations and special pathological entities like salivary gland tumors [27,28] . A series of 606 upper
and lower alveolar SCCs reported 37% of cervical metastasis and 19% of harbored occult disease in elective
neck dissections. Lymph node involvement at level II to V carried shorter survival than negative lymph node
[19]
involvement . A series of 347 cancers of the upper and lower gums that had an elective neck dissection rate
of 58% found occult disease in 5.6%. Neck recurrence was found in 9% of the whole group. Ipsilateral and
contralateral neck node involvement predicted cervical recurrence. Positive neck lymph nodes, tumor stage,
and involved soft-tissue margins were significant covariates in survival prediction; clinical stage remained
[29]
significant in multivariate analysis . A series of 252 cases of palate SCC including 62 in the specific region