Page 50 - Read Online
P. 50
Page 6 of 15 Otsuka et al. Hepatoma Res 2021;7:5 I http://dx.doi.org/10.20517/2394-5079.2020.112
A B
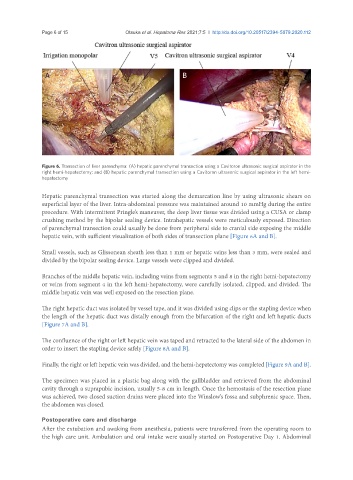
Figure 6. Transection of liver parenchyma: (A) hepatic parenchymal transection using a Cavitoron ultrasonic surgical aspirator in the
right hemi-hepatectomy; and (B) hepatic parenchymal transection using a Cavitoron ultrasonic surgical aspirator in the left hemi-
hepatectomy
Hepatic parenchymal transection was started along the demarcation line by using ultrasonic shears on
superficial layer of the liver. Intra-abdominal pressure was maintained around 10 mmHg during the entire
procedure. With intermittent Pringle’s maneuver, the deep liver tissue was divided using a CUSA or clamp
crushing method by the bipolar sealing device. Intrahepatic vessels were meticulously exposed. Direction
of parenchymal transection could usually be done from peripheral side to cranial side exposing the middle
hepatic vein, with sufficient visualization of both sides of transection plane [Figure 6A and B].
Small vessels, such as Glissonean sheath less than 1 mm or hepatic veins less than 3 mm, were sealed and
divided by the bipolar sealing device. Large vessels were clipped and divided.
Branches of the middle hepatic vein, including veins from segments 5 and 8 in the right hemi-hepatectomy
or veins from segment 4 in the left hemi-hepatectomy, were carefully isolated, clipped, and divided. The
middle hepatic vein was well exposed on the resection plane.
The right hepatic duct was isolated by vessel tape, and it was divided using clips or the stapling device when
the length of the hepatic duct was distally enough from the bifurcation of the right and left hepatic ducts
[Figure 7A and B].
The confluence of the right or left hepatic vein was taped and retracted to the lateral side of the abdomen in
order to insert the stapling device safely [Figure 8A and B].
Finally, the right or left hepatic vein was divided, and the hemi-hepatectomy was completed [Figure 9A and B].
The specimen was placed in a plastic bag along with the gallbladder and retrieved from the abdominal
cavity through a suprapubic incision, usually 5-8 cm in length. Once the hemostasis of the resection plane
was achieved, two closed suction drains were placed into the Winslow’s fossa and subphrenic space. Then,
the abdomen was closed.
Postoperative care and discharge
After the extubation and awaking from anesthesia, patients were transferred from the operating room to
the high care unit. Ambulation and oral intake were usually started on Postoperative Day 1. Abdominal