Page 67 - Read Online
P. 67
Figure 3: Case 9: (a) Sensate ALT flap, LCFN included; (b) intraoperative
sizable septocutaneous perforator (TBLCFAP-s) was 18 cm from ASIS as
determined preoperatively by MDCTA; (c) 8 weeks postoperative showing
well settled sensate ALT flap; (d) posttraumatic heel defect with exposed
calcaneus. ALT: anterolateral thigh; LCFN: lateral cutaneous femoral nerve;
ASIS: anterior superior iliac spine; MDCTA: multi-detector row computed
tomography angiography; TBLCFAP-s: septocutaneous perforator from
transverse branch of lateral circumflex femoral artery through spectrum
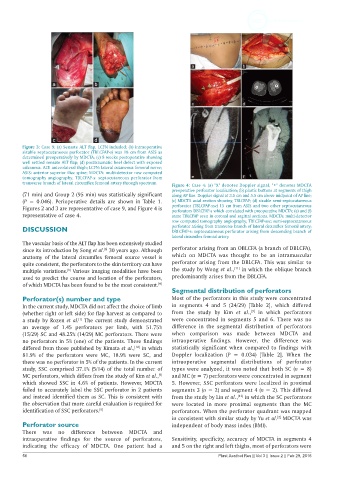
Figure 4: Case 4: (a) "X" denotes Doppler signal, "•" denotes MDCTA
preoperative perforator localization; (b) plastic buttons at segments of thigh
(71 min) and Group 2 (95 min) was statistically significant along AP line. Doppler signal at 3.5 cm and 5.5 cm above midpoint of AP line;
(P = 0.046). Perioperative details are shown in Table 1. (c) MDCTA axial section showing TBLCFAP; (d) sizable semi-septocutaneous
Figures 2 and 3 are representative of case 9, and Figure 4 is perforator (TBLCFAP-ssc) 15 cm from ASIS and two other septocutaneous
perforators DBLCFAP-s which correlated with preoperative MDCTA; (e) and (f)
representative of case 4. same TBLCFAP seen in coronal and sagittal sections. MDCTA: multi-detector
row computed tomography angiography; TBLCFAP-ssc: semi-septocutaneous
DISCUSSION perforator arising from transverse branch of lateral circumflex femoral artery;
DBLCFAP-s: septocutaneous perforator arising from descending branch of
lateral circumflex femoral artery
The vascular basis of the ALT flap has been extensively studied
[6]
since its introduction by Song et al. 30 years ago. Although perforator arising from an OBLCFA (a branch of DBLCFA),
anatomy of the lateral circumflex femoral source vessel is which on MDCTA was thought to be an intramuscular
quite consistent, the perforators to the skin territory can have perforator arising from the DBLCFA. This was similar to
[11]
multiple variations. Various imaging modalities have been the study by Wong et al., in which the oblique branch
[9]
used to predict the course and location of the perforators, predominantly arises from the DBLCFA.
of which MDCTA has been found to be the most consistent. [9]
Segmental distribution of perforators
Perforator(s) number and type Most of the perforators in this study were concentrated
In the current study, MDCTA did not affect the choice of limb in segments 4 and 5 (24/29) [Table 2], which differed
[9]
(whether right or left side) for flap harvest as compared to from the study by Kim et al., in which perforators
a study by Rozen et al. The current study demonstrated were concentrated in segments 5 and 6. There was no
[1]
an average of 1.45 perforators per limb, with 51.75% difference in the segmental distribution of perforators
(15/29) SC and 48.25% (14/29) MC perforators. There were when comparison was made between MDCTA and
no perforators in 5% (one) of the patients. These findings intraoperative findings. However, the difference was
differed from those published by Kimata et al., in which statistically significant when compared to findings with
[10]
81.9% of the perforators were MC, 18.9% were SC, and Doppler localization (P = 0.034) [Table 2]. When the
there was no perforator in 5% of the patients. In the current intraoperative segmental distributions of perforator
study, SSC comprised 37.1% (5/14) of the total number of types were analyzed, it was noted that both SC (n = 8)
[9]
MC perforators, which differs from the study of Kim et al., and MC (n = 7) perforators were concentrated in segment
which showed SSC in 4.6% of patients. However, MDCTA 5. However, SSC perforators were localized in proximal
failed to accurately label the SSC perforator in 2 patients segments 3 (n = 2) and segment 4 (n = 2). This differed
and instead identified them as SC. This is consistent with from the study by Lin et al., in which the SC perforators
[12]
the observation that more careful evaluation is required for were located in more proximal segments than the MC
identification of SSC perforators. [9] perforators. When the perforator quadrant was mapped
in consistent with similar study by Yu et al. MDCTA was
[2]
Perforator source independent of body mass index (BMI).
There was no difference between MDCTA and
intraoperative findings for the source of perforators, Sensitivity, specificity, accuracy of MDCTA in segments 4
indicating the efficacy of MDCTA. One patient had a and 5 on the right and left thighs, most of perforators were
56 Plast Aesthet Res || Vol 3 || Issue 2 || Feb 29, 2016