Page 66 - Read Online
P. 66
closer to the mean in the MDCTA-intraoperative plot, between the mean VAS of Group 1 (2.1) and Group 2 (2.5)
indicating a good agreement in the locations of the was not statistically significant (P = 0.63). The difference
perforators as compared to the Doppler-intraoperative between mean flap harvest time of Group 1 (87.5 min)
plot which was dispersed away from the mean. and Group 2 (117.5 min) was not statistically significant
(P = 0.28). However, operator bias cannot be ruled out.
Surgeons’ stress levels Surgeon A (chief surgeon) performed an equal number of
A VAS was used to record the level of stress experienced surgeries (five) in each group, of which two cases in each
by the surgeon during flap harvest. The difference group required an intramuscular perforator dissection
for perforators arising from the DLBCFA. The difference
between mean flap harvest time for Surgeon A in Group 1
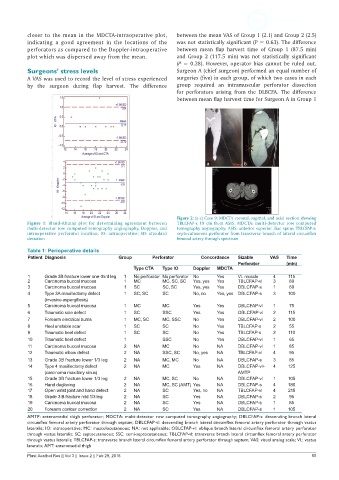
Figure 2: (a-c) Case 9: MDCTA coronal, sagittal, and axial section showing
Figure 1: Bland-Altman plot for determining agreement between TBLCFAP-s 18 cm from ASIS. MDCTA: multi-detector row computed
multi-detector row computed tomography angiography, Doppler, and tomography angiography; ASIS: anterior superior iliac spine; TBLCFAP-s:
intraoperative perforator location. IO: intraoperative; SD: standard septocutaneous perforator from transverse branch of lateral circumflex
deviation femoral artery through spectrum
Table 1: Perioperative details
Patient Diagnosis Group Perforator Concordance Sizable VAS Time
Perforator (min)
Type CTA Type IO Doppler MDCTA
1 Grade 3B fracture lower one-third leg 1 No perforator No perforator No Yes VL muscle 4 115
2 Carcinoma buccal mucosa 1 MC MC, SC, SC Yes, yes Yes TBLCFAP-vl 3 80
3 Carcinoma buccal mucosa 1 SC SC, SC Yes, yes Yes DBLCFAP-s 1 60
4 Type 3A maxillectomy defect 1 SC, SC SC No, no Yes, yes DBLCFAP-s 3 100
(invasive aspergillosis)
5 Carcinoma buccal mucosa 1 MC MC Yes Yes DBLCFAP-vl 1 75
6 Traumatic sole defect 1 SC SSC Yes Yes OBLCFAP-vl 2 115
7 Forearm electrical burns 1 MC, SC MC, SSC No Yes DBLCFAP-vl 2 100
8 Heel unstable scar 1 SC SC No Yes TBLCFAP-s 2 55
9 Traumatic heel defect 1 SC SC No Yes TBLCFAP-s 2 110
10 Traumatic heel defect 1 SSC No Yes DBLCFAP-vl 1 65
11 Carcinoma buccal mucosa 2 NA MC No NA DBLCFAP-vl 1 85
12 Traumatic elbow defect 2 NA SSC, SC No, yes NA TBLCFAP-vl 4 95
13 Grade 3B fracture lower 1/3 leg 2 NA MC, MC No NA DBLCFAP-s 3 85
14 Type 4 maxillectomy defect 2 NA MC Yes NA DBLCFAP-vl+ 4 125
(carcinoma maxillary sinus) AMTP
15 Grade 3B fracture lower 1/3 leg 2 NA MC, SC No NA DBLCFAP-vl 1 105
16 Hand degloving 2 NA MC, SC (AMT) Yes NA DBLCFAP-s 4 180
17 Open wrist joint and hand defect 2 NA SC Yes, no NA TBLCFAP-vl 4 215
18 Grade 3 B fracture mid 1/3 leg 2 NA SC Yes NA DBLCFAP-s 2 95
19 Carcinoma buccal mucosa 2 NA SC Yes NA DBLCFAP-s 1 85
20 Forearm contour correction 2 NA SC Yes NA DBLCFAP-s 1 105
AMTP: anteromedial thigh perforator; MDCTA: multi-detector row computed tomography angiography; DBLCFAP-s: descending branch lateral
circumflex femoral artery perforator through septum; DBLCFAP-vl: descending branch lateral circumflex femoral artery perforator through vastus
lateralis; IO: intraoperative; MC: musculocutaneous; NA: not applicable; OBLCFAP-vl: oblique branch lateral circumflex femoral artery perforator
through vastus lateralis; SC: septocutaneous; SSC: semi-septocutaneous; TBLCFAP-vl: transverse branch lateral circumflex femoral artery perforator
through vastus lateralis; TBLCFAP-s: transverse branch lateral circumflex femoral artery perforator through septum; VAS: visual analog scale; VL: vastus
lateralis; AMT: anteromedial thigh
Plast Aesthet Res || Vol 3 || Issue 2 || Feb 29, 2016 55