Page 58 - Read Online
P. 58
Chen et al. Contralateral cerebral ischemia after MMD bypass
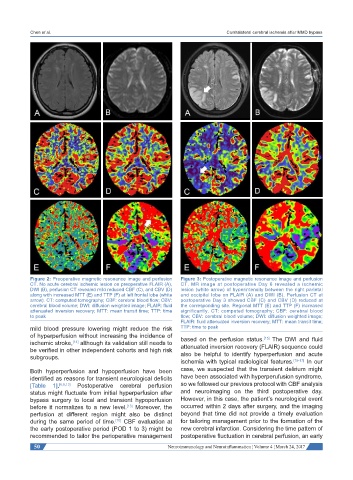
Figure 2: Preoperative magnetic resonance image and perfusion Figure 3: Postoperative magnetic resonance image and perfusion
CT. No acute cerebral ischemic lesion on preoperative FLAIR (A), CT. MR image at postoperative Day 6 revealed a ischemic
DWI (B), perfusion CT revealed mild reduced CBF (C), and CBV (D) lesion (white arrow) of hyperintensity between the right parietal
along with increased MTT (E) and TTP (F) at left frontal lobe (white and occipital lobe on FLAIR (A) and DWI (B). Perfusion CT at
arrow). CT: computed tomography; CBF: cerebral blood flow; CBV: postoperative Day 3 showed CBF (C) and CBV (D) reduced at
cerebral blood volume; DWI: diffusion weighted image; FLAIR: fluid the corresponding site. Regional MTT (E) and TTP (F) increased
attenuated inversion recovery; MTT: mean transit time; TTP: time significantly. CT: computed tomography; CBF: cerebral blood
to peak flow; CBV: cerebral blood volume; DWI: diffusion weighted image;
FLAIR: fluid attenuated inversion recovery; MTT: mean transit time;
mild blood pressure lowering might reduce the risk TTP: time to peak
of hyperperfusion without increasing the incidence of based on the perfusion status. The DWI and fluid
[15]
ischemic stroke, although its validation still needs to attenuated inversion recovery (FLAIR) sequence could
[14]
be verified in other independent cohorts and high risk also be helpful to identify hyperperfusion and acute
subgroups.
ischemia with typical radiological features. [15-17] In our
Both hyperperfusion and hypoperfusion have been case, we suspected that the transient delirium might
identified as reasons for transient neurological deficits have been associated with hyperperufusion syndrome,
[Table 1]. [6,8,13] Postoperative cerebral perfusion so we followed our previous protocol with CBF analysis
status might fluctuate from initial hyperperfusion after and neuroimaging on the third postoperative day.
bypass surgery to local and transient hypoperfusion However, in this case, the patient’s neurological event
before it normalizes to a new level. Moreover, the occurred within 2 days after surgery, and the imaging
[13]
perfusion at different region might also be distinct beyond that time did not provide a timely evaluation
during the same period of time. CBF evaluation at for tailoring management prior to the formation of the
[10]
the early postoperative period (POD 1 to 3) might be new cerebral infarction. Considering the time pattern of
recommended to tailor the perioperative management postoperative fluctuation in cerebral perfusion, an early
50 Neuroimmunology and Neuroinflammation ¦ Volume 4 ¦ March 24, 2017