Page 56 - Read Online
P. 56
Chen et al. Contralateral cerebral ischemia after MMD bypass
In MMD with unilateral STA-MCA bypass, symptomatic parietal and occipital lobes were not well developed.
cerebral ischemia in the contralateral hemisphere Preoperative perfusion CT also indicated impaired
more commonly occurs in patients with advanced perfusion in the aforementioned area [Figures 1 and 2].
stage (Suzuki stage 4 to 6), PCA involvement and These angioarchitecture and perfusion features might
postoperative hypotension on postoperative Day be the underlying factors contributing to the focal
(POD) 1 and Day 2. Advanced Suzuki stage and ischemic deterioration after stress, including surgery
[7]
PCA involvement indicate the progression of MMD. and delirium. Therefore, intensive perioperative care
[11]
In these patients, cerebral hemodynamics might be should be recommended for these MMD patients with
unstable and more susceptible to cerebral infarction high risk factors [Table 1]. Real-time monitoring of
[12]
after fluctuations of perfusion during the perioperative the cerebral blood flow (CBF) showed that the regional
period. The patient in this case had a bilateral CBF after revascularization followed a variable pattern
[7]
advanced stage of MMD (stage 4 for the left and stage with significant decreases between 12 h and 24 h after
3 for the right) with right PCA involvement [Figure 1]. surgery and at 36 h after surgery. This CBF pattern
[13]
Although the unilateral direct revascularization might correlated with the onset of a transient neurological
directly influence the blood flow of the contralateral event in our case and suggested a careful blood
hemisphere through collaterals, the collaterals from pressure management during the early postoperative
the contralateral side, in the present case, were poorly period. In addition, rather than arbitrarily maintaining
developed and were mainly around the midline, which the blood pressure between certain parameters, the
might not explain the ischemia of the remote convexity blood pressure management should be referenced to
[Figure 1]. Retrospective analysis of DSA suggested the preoperative level to avoid a rapid decrease from
that the right PCA collaterals to the watershed between the baseline. Recent data suggested that prophylactic
[7]
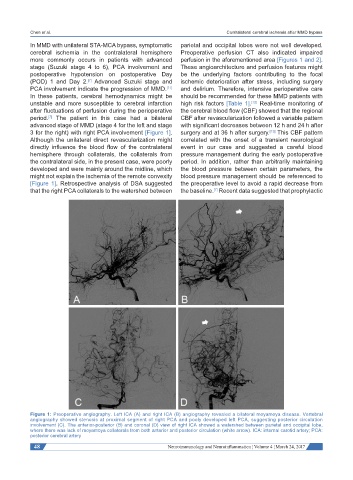
Figure 1: Preoperative angiography. Left ICA (A) and right ICA (B) angiography revealed a bilateral moyamoya disease. Vertebral
angiography showed stenosis at proximal segment of right PCA and pooly developed left PCA, suggesting posterior circulation
involvement (C). The anterior-posterior (B) and coronal (D) view of right ICA showed a watershed between parietal and occipital lobe,
where there was lack of moyamoya collaterals from both anterior and posterior circulation (white arrow). ICA: internal carotid artery; PCA:
posterior cerebral artery
48 Neuroimmunology and Neuroinflammation ¦ Volume 4 ¦ March 24, 2017