Page 127 - Read Online
P. 127
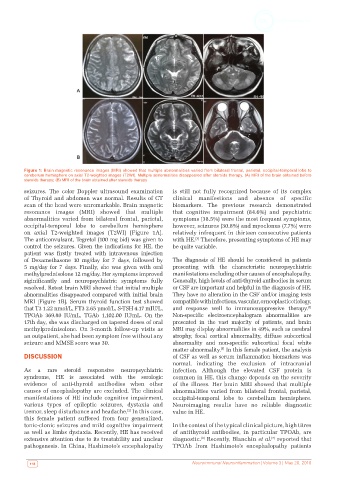
Figure 1: Brain magnetic resonance images (MRI) showed that multiple abnormalities varied from bilateral frontal, parietal, occipital-temporal lobe to
cerebellum hemisphere on axial T2-weighted images (T2WI). Multiple abnormalities disappeared after steroids therapy. (A) MRI of the brain obtained before
steroids therapy; (B) MRI of the brain obtained after steroids therapy
seizures. The color Doppler ultrasound examination is still not fully recognized because of its complex
of Thyroid and abdomen was normal. Results of CT clinical manifestions and absence of specific
scan of the head were unremarkable. Brain magnetic biomarkers. The previous research demonstrated
resonance images (MRI) showed that multiple that cognitive impairment (84.6%) and psychiatric
abnormalities varied from bilateral frontal, parietal, symptoms (38.5%) were the most frequent symptoms,
occipital-temporal lobe to cerebellum hemisphere however, seizures (30.8%) and myoclonus (7.7%) were
on axial T2-weighted images (T2WI) [Figure 1A]. relatively infrequent in thirteen consecutive patients
The anticonvulsant, Tegretol (100 mg bid) was given to with HE. Therefore, presenting symptoms of HE may
[3]
control the seizures. Given the indications for HE, the be quite variable.
patient was firstly treated with intravenous injection
of Dexamethasone 10 mg/day for 7 days, followed by The diagnosis of HE should be considered in patients
5 mg/day for 7 days. Finally, she was given with oral presenting with the characteristic neuropsychiatric
methylprednisolone 12 mg/day. Her symptoms improved manifestations excluding other causes of encephalopathy.
siginificantly and neuropsychiatric symptoms fully Generally, high levels of anti-thyroid antibodies in serum
resolved. Retest brain MRI showed that initial multiple or CSF are important and helpful in the diagnosis of HE.
abnormalities disappeared compared with initial brain They have no alteration in the CSF and/or imaging tests
MRI [Figure 1B]. Serum thyroid function test showed compatible with infectious, vascular, or neoplastic etiology,
[4]
that T3 1.22 nmol/L, FT3 2.65 pmol/L, S-TSH 4.17 mIU/L, and response well to immunosuppressive therapy.
TPOAb 369.80 IU/mL, TGAb 1,102.00 IU/mL. On the Non-specific electroencephalogram abnormalities are
17th day, she was discharged on tapered doses of oral presented in the vast majority of patients, and brain
methylprednisolone. On 3-month follow-up visits as MRI may display abnormalities in 49%, such as cerebral
an outpatient, she had been symptom free without any atrophy, focal cortical abnormality, diffuse subcortical
seizure and MMSE score was 30. abnormality and non-specific subcortical focal white
matter abnormality. In this female patient, the analysis
[5]
DISCUSSION of CSF as well as serum inflammation biomarkers was
normal, indicating the exclusion of intracranial
As a rare steroid responsive neuropsychiatric infection. Although the elevated CSF protein is
syndrome, HE is associated with the serologic common in HE, this change depends on the severity
evidence of anti-thyroid antibodies when other of the illness. Her brain MRI showed that multiple
causes of encephalopathy are excluded. The clinical abnormalities varied from bilateral frontal, parietal,
manifestations of HE include cognitive impairment, occipital-temporal lobe to cerebellum hemisphere.
various types of epileptic seizures, dystaxia and Neuroimaging results have no reliable diagnostic
tremor, sleep disturbance and headache. In this case, value in HE.
[2]
this female patient suffered from four generalized,
tonic-clonic seizures and mild cognitive impairment In the context of the typical clinical picture, high titres
as well as limbs dystaxia. Recently, HE has received of antithyroid antibodies, in particular TPOAb, are
extensive attention due to its treatability and unclear diagnostic. Recently, Blanchin et al. reported that
[7]
[6]
pathogenesis. In China, Hashimoto’s encephalopathy TPOAb from Hashimoto’s encephalopathy patients
118 Neuroimmunol Neuroinflammation | Volume 3 | May 20, 2016