Page 71 - Read Online
P. 71
Zavridis et al. Radio frequency neurolysis for pain reduction
Comparing the self-reported pain scores of ongoing tissue damage) or neuropathic (caused by
questionnaires prior to treatment (mean value 9.50 damage or dysfunction in the nervous system). [2,3] The
NRS units, range 8-10 NRS units) and at 6 months WHO analgesic ladder has three steps for acute pain,
post treatment (mean value 3.27 NRS units range chronic pain without control, or acute crises of chronic
2-6 NRS units), there was a mean decrease of 6.23 pain. In step 1, nonopioids, analgesics, and NSAIDs
NRS units in terms of pain reduction and life quality are administered to the patient. In step 2, weak
improvement [Figure 5]. Overall mobility improved in opioids can be added to the treatment regime. In step
18/18 (100%) patients. 3, methadone or strong opioids can be administered
orally or by means of a transdermal patch.
DISCUSSION
Unfortunately, conservative therapy does not
Cancer pain has direct implications for patients’ quality adequately reduce pain in the vast majority of oncologic
of life. Cancer pain can be classified as nociceptive patients (56% to 82.3%). [2,3] On the other hand,
(described as somatic or visceral and caused by numerous studies in the literature report significant
pain reduction post chemical or thermal neurolysis. [13-16]
Papadopoulos et al., who conducted treatment with
[17]
radiofrequency ablation of splanchnic nerves on 35
patients with end-stage pancreatic abdominal cancer
pain refractory to conservative treatment, reported
significant decrease in pain scores and consumption
of opioids and significant improvement in the patient
quality of life during a follow-up period of 6 months.
Our study included patients with a diversity of malignant
substrate, evaluating the efficacy of RF neurolysis in
celiac and splanchnic plexus (n = 9), in the thorax (n =
1), in the lumbar region (n = 2), in superior hypogastric
plexus (n = 5), and in the stellate ganglion (n = 5).
The results of our study (statistically significant mean
decrease of 6.23 NVS units on terms of pain reduction
and life quality improvement) are in agreement with the
previously mentioned success rates.
Percutaneous neurolysis has been reported as a safe
procedure with a low complications rate. The most
commonly reported complications include transient
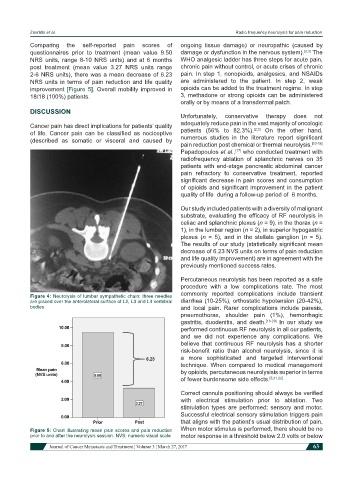
Figure 4: Neurolysis of lumbar sympathetic chain: three needles
are placed over the anterolateral surface of L2, L3 and L4 vertebral diarrhea (10-25%), orthostatic hypotension (20-42%),
bodies and local pain. Rarer complications include paresis,
pneumothorax, shoulder pain (1%), hemorrhagic
gastritis, duodenitis, and death. [18-20] In our study we
performed continuous RF neurolysis in all our patients,
and we did not experience any complications. We
believe that continuous RF neurolysis has a shorter
risk-benefit ratio than alcohol neurolysis, since it is
a more sophisticated and targeted interventional
technique. When compared to medical management
by opioids, percutaneous neurolysisis superior in terms
of fewer burdensome side effects. [5,21,22]
Correct cannula positioning should always be verified
with electrical stimulation prior to ablation. Two
stimulation types are performed: sensory and motor.
Successful electrical sensory stimulation triggers pain
that aligns with the patient’s usual distribution of pain.
Figure 5: Chart illustrating mean pain scores and pain reduction When motor stimulus is performed, there should be no
prior to and after the neurolysis session. NVS: numeric visual scale motor response in a threshold below 2.0 volts or below
Journal of Cancer Metastasis and Treatment ¦ Volume 3 ¦ March 27, 2017 63