Page 70 - Read Online
P. 70
Zavridis et al. Radio frequency neurolysis for pain reduction
of interest, 20 G trocar(s) was (were) percutaneously the superior articular process of S1 or via transdiscal
inserted and advanced. The final trocar position was access. Thoracic neurolysis was performed with the
verified with CT scan post contrast medium injection. needles placed at the space between vertebral body
(lateral aspect) and pleura at T2 and T3 levels.
For the celiac plexus neurolysis, a posterior transcrural
approach was used, with needles passing through Coaxially, the RF electrode was then inserted [Figures 2-4].
the diaphragmatic crura in route to the celiac plexus Motor and sensory tests were performed to verify
anterolateral to the aorta. For the neurolysis of the electrode’s correct position near the sensory
the splanchnic nerves, a retrocrural approach was nerve segment and away from the motor root. Upon
performed with the needles remaining posterior to satisfactory test results, two CRF ablation sessions
the diaphragmatic crura and placed at the level of L1 were performed at 80 °C, with total duration time
vertebral body (cephalad half) and at midportion of T12 of 90 s each. All patients were closely observed
vertebral body. For the lumbar plexus neurolysis, two or postoperatively for pain, sensory and motor deficits, as
three needles were placed over the transverse process well as for vital signs. Patients remained in the hospital
of L2, L3 and L4 vertebrae, respectively, with the needle overnight for hydration and observation and exited the
tip at the anteromedial vertebral body surface where morning after the procedure.
the lumbar sympathetic block lies. For the superior
hypogastric neurolysis, the needle was placed at the Outcome measures
anterolateral surface of L5-S1 intervertebral disc, either Pain assessment was performed using the Numeric
via posterolateral access through the sacral ala and Rating Scale (NRS, 0-10) questionnaire and Brief Pain
Inventory (Short Form) questionnaire for reviewing
quality of life. The questionnaires were recorded
[19]
before the treatment, one week after treatment, and at
the last follow-up (average follow-up 6 months).
RESULTS
Twenty-two patients were studied, all suffering from
cancer pain refractory to systemic therapy with opioids
and adjuvant drugs. All patients completed the follow-
up of six months.
Median procedure time was 44 min. Median number of
CT scans, performed to control correct positioning of
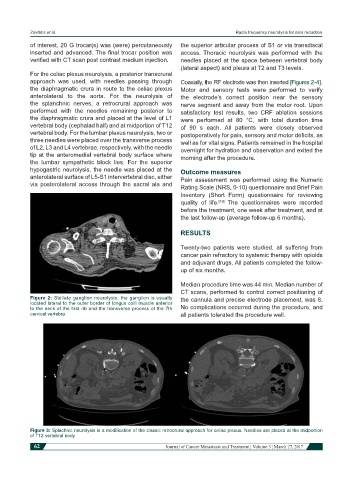
Figure 2: Stellate ganglion neurolysis: the ganglion is usually the cannula and precise electrode placement, was 8.
located lateral to the outer border of longus colli muscle anterior
to the neck of the first rib and the transverse process of the 7th No complications occurred during the procedure, and
cervical vertebra all patients tolerated the procedure well.
Figure 3: Splachnic neurolysis is a modification of the classic retrocrural approach for celiac plexus. Needles are placed at the midportion
of T12 vertebral body
62 Journal of Cancer Metastasis and Treatment ¦ Volume 3 ¦ March 27, 2017