Page 156 - Read Online
P. 156
Ieni et al. Colonic metastasis by a uterine LCNEC
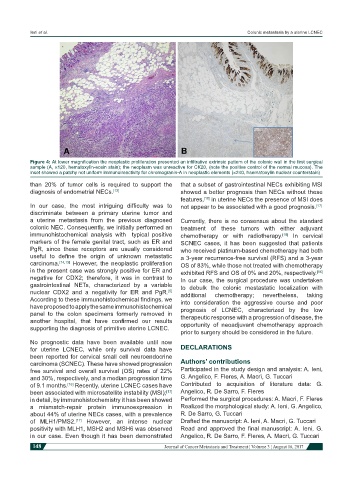
Figure 4: At lower magnification the neoplastic proliferation presented an infiltrative extrinsic pattern of the colonic wall in the first surgical
sample (A, ×120, hematoxylin-eosin stain); the neoplasm was unreactive for CK20, (note the positive control of the normal mucosa). The
inset showed a patchy not uniform immunoireactivity for chromogranin-A in neoplastic elements (×240, haematoxylin nuclear counterstain)
than 20% of tumor cells is required to support the that a subset of gastrointestinal NECs exhibiting MSI
diagnosis of endometrial NECs. [13] showed a better prognosis than NECs without these
features, in uterine NECs the presence of MSI does
[18]
In our case, the most intriguing difficulty was to not appear to be associated with a good prognosis. [17]
discriminate between a primary uterine tumor and
a uterine metastasis from the previous diagnosed Currently, there is no consensus about the standard
colonic NEC. Consequently, we initially performed an treatment of these tumors with either adjuvant
immunohistochemical analysis with typical positive chemotherapy or with radiotherapy. In cervical
[19]
markers of the female genital tract, such as ER and SCNEC cases, it has been suggested that patients
PgR, since these receptors are usually considered who received platinum-based chemotherapy had both
useful to define the origin of unknown metastatic a 3-year recurrence-free survival (RFS) and a 3-year
carcinoma. [14,15] However, the neoplastic proliferation OS of 83%, while those not treated with chemotherapy
in the present case was strongly positive for ER and exhibited RFS and OS of 0% and 20%, respectively.
[16]
negative for CDX2; therefore, it was in contrast to In our case, the surgical procedure was undertaken
gastrointestinal NETs, characterized by a variable to debulk the colonic mestastatic localization with
nuclear CDX2 and a negativity for ER and PgR. additional chemotherapy; nevertheless, taking
[5]
According to these immunohistochemical findings, we into consideration the aggressive course and poor
have proposed to apply the same immunohistochemical prognosis of LCNEC, characterized by the low
panel to the colon specimens formerly removed in therapeutic response with a progression of disease, the
another hospital, that have confirmed our results opportunity of neoadjuvant chemotherapy approach
supporting the diagnosis of primitive uterine LCNEC.
prior to surgery should be considered in the future.
No prognostic data have been available until now
for uterine LCNEC, while only survival data have DECLARATIONS
been reported for cervical small cell neuroendocrine
carcinoma (SCNEC). These have showed progression Authors’ contributions
free survival and overall survival (OS) rates of 22% Participated in the study design and analysis: A. Ieni,
and 30%, respectively, and a median progression time G. Angelico, F. Fleres, A. Macrì, G. Tuccari
of 9.1 months. Recently, uterine LCNEC cases have Contributed to acquisition of literature data: G.
[16]
been associated with microsatellite instability (MSI); Angelico, R. De Sarro, F. Fleres
[17]
in detail, by immunohistochemistry it has been showed Performed the surgical procedures: A. Macrì, F. Fleres
a mismatch-repair protein immunoexpression in Realized the morphological study: A. Ieni, G. Angelico,
about 44% of uterine NECs cases, with a prevalence R. De Sarro, G. Tuccari
of MLH1/PMS2. However, an intense nuclear Drafted the manuscript: A. Ieni, A. Macrì, G. Tuccari
[17]
positivity with MLH1, MSH2 and MSH6 was observed Read and approved the final manuscript: A. Ieni, G.
in our case. Even though it has been demonstrated Angelico, R. De Sarro, F. Fleres, A. Macrì, G. Tuccari
148 Journal of Cancer Metastasis and Treatment ¦ Volume 3 ¦ August 16, 2017