Page 148 - Read Online
P. 148
Agrawal et al. Challenging treatment of huge fibromatosis
breathlessness for 2 months. Chest X-ray (PA view) 28 fractions was delivered at the rate of 1.8 Gy per
reported dense homogeneity over the right middle fraction, 5 fractions per week for 5 weeks to clinical
and lower zones. A computed tomography (CT) scan target volume (CTV) by image guided radiotherapy
of thorax and abdomen with contrast showed a large technique. The doses delivered to CTV in the axial,
pleural based mass of approximately 12 cm × 13 cm coronal and saggital sections are represented in
× 19 cm in the right thoracic cavity, probably arising Figures 3-5. Adjacent normal structures (right lung,
from right chest wall, extending into the mediastinum,
with smooth indentation on pericardium and superior heart, right breast, liver) were given dose constraints.
vena cava with no evidence of rib destruction We achieved a volume of 20 Gy (V20) as follows,
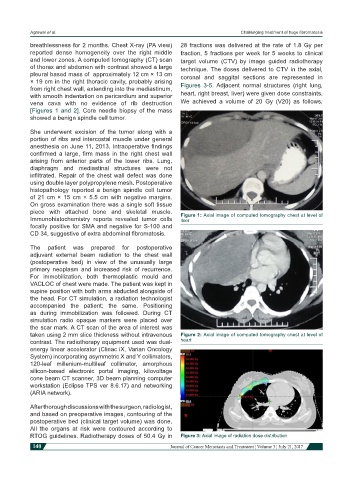
[Figures 1 and 2]. Core needle biopsy of the mass
showed a benign spindle cell tumor.
She underwent excision of the tumor along with a
portion of ribs and intercostal muscle under general
anesthesia on June 11, 2013. Intraoperative findings
confirmed a large, firm mass in the right chest wall
arising from anterior parts of the lower ribs. Lung,
diaphragm and mediastinal structures were not
infiltrated. Repair of the chest wall defect was done
using double layer polypropylene mesh. Postoperative
histopathology reported a benign spindle cell tumor
of 21 cm × 15 cm × 5.5 cm with negative margins.
On gross examination there was a single soft tissue
piece with attached bone and skeletal muscle. Figure 1: Axial image of computed tomography chest at level of
Immunohistochemistry reports revealed tumor cells liver
focally positive for SMA and negative for S-100 and
CD 34, suggestive of extra abdominal fibromatosis.
The patient was prepared for postoperative
adjuvant external beam radiation to the chest wall
(postoperative bed) in view of the unusually large
primary neoplasm and increased risk of recurrence.
For immobilization, both thermoplastic mould and
VACLOC of chest were made. The patient was kept in
supine position with both arms abducted alongside of
the head. For CT simulation, a radiation technologist
accompanied the patient; the same. Positioning
as during immobilization was followed. During CT
simulation radio opaque markers were placed over
the scar mark. A CT scan of the area of interest was
taken using 2 mm slice thickness without intravenous Figure 2: Axial image of computed tomography chest at level of
contrast. The radiotherapy equipment used was dual- heart
energy linear accelerator (Clinac iX, Varian Oncology
System) incorporating asymmetric X and Y collimators,
120-leaf millenium-multileaf collimator, amorphous
silicon-based electronic portal imaging, kilovoltage
cone beam CT scanner, 3D beam planning computer
workstation (Eclipse TPS ver 8.6.17) and networking
(ARIA network).
After thorough discussions with the surgeon, radiologist,
and based on preoperative images, contouring of the
postoperative bed (clinical target volume) was done.
All the organs at risk were contoured according to
RTOG guidelines. Radiotherapy doses of 50.4 Gy in Figure 3: Axial image of radiation dose distribution
140 Journal of Cancer Metastasis and Treatment ¦ Volume 3 ¦ July 21, 2017