Page 91 - Read Online
P. 91
Sarkar et al. Predictors of survival in HCC treatment
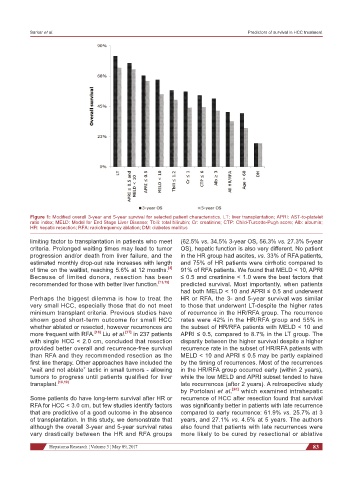
Figure 1: Modified overall 3-year and 5-year survival for selected patient characteristics. LT: liver transplantation; APRI: AST-to-platelet
ratio index; MELD: Model for End Stage Liver Disease; Tbili: total bilirubin; Cr: creatinine; CTP: Child-Turcotte-Pugh score; Alb: albumin;
HR: hepatic resection; RFA: radiofrequency ablation; DM: diabetes mellitus
limiting factor to transplantation in patients who meet (62.5% vs. 34.5% 3-year OS, 56.3% vs. 27.3% 5-year
criteria. Prolonged waiting times may lead to tumor OS), hepatic function is also very different. No patient
progression and/or death from liver failure, and the in the HR group had ascites, vs. 33% of RFA patients,
estimated monthly drop-out rate increases with length and 75% of HR patients were cirrhotic compared to
[4]
of time on the waitlist, reaching 5.6% at 12 months. 91% of RFA patients. We found that MELD < 10, APRI
Because of limited donors, resection has been ≤ 0.5 and creatinine < 1.0 were the best factors that
recommended for those with better liver function. [13,15] predicted survival. Most importantly, when patients
had both MELD < 10 and APRI ≤ 0.5 and underwent
Perhaps the biggest dilemma is how to treat the HR or RFA, the 3- and 5-year survival was similar
very small HCC, especially those that do not meet to those that underwent LT-despite the higher rates
minimum transplant criteria. Previous studies have of recurrence in the HR/RFA group. The recurrence
shown good short-term outcome for small HCC rates were 42% in the HR/RFA group and 55% in
whether ablated or resected, however recurrences are the subset of HR/RFA patients with MELD < 10 and
more frequent with RFA. [16] Liu et al. [17] in 237 patients APRI ≤ 0.5, compared to 8.7% in the LT group. The
with single HCC < 2.0 cm, concluded that resection disparity between the higher survival despite a higher
provided better overall and recurrence-free survival recurrence rate in the subset of HR/RFA patients with
than RFA and they recommended resection as the MELD < 10 and APRI ≤ 0.5 may be partly explained
first line therapy. Other approaches have included the by the timing of recurrences. Most of the recurrences
“wait and not ablate” tactic in small tumors - allowing in the HR/RFA group occurred early (within 2 years),
tumors to progress until patients qualified for liver while the low MELD and APRI subset tended to have
transplant. [18,19] late recurrences (after 2 years). A retrospective study
by Portolani et al. [20] which examined intrahepatic
Some patients do have long-term survival after HR or recurrence of HCC after resection found that survival
RFA for HCC < 3.0 cm, but few studies identify factors was significantly better in patients with late recurrence
that are predictive of a good outcome in the absence compared to early recurrence: 61.9% vs. 25.7% at 3
of transplantation. In this study, we demonstrate that years, and 27.1% vs. 4.5% at 5 years. The authors
although the overall 3-year and 5-year survival rates also found that patients with late recurrences were
vary drastically between the HR and RFA groups more likely to be cured by resectional or ablative
Hepatoma Research ¦ Volume 3 ¦ May 09, 2017 83