Page 181 - Read Online
P. 181
Isetani et al. Laparoscopic surgery for gallbladder carcinoma
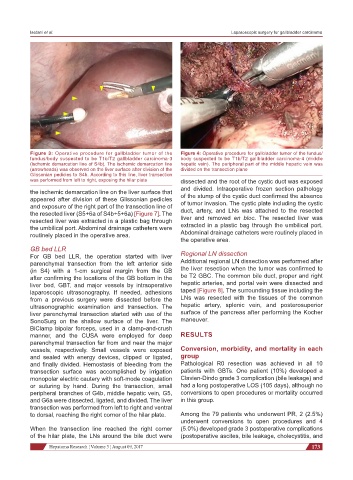
Figure 3: Operative procedure for gallbladder tumor of the Figure 4: Operative procedure for gallbladder tumor of the fundus/
fundus/body suspected to be T1b/T2 gallbladder carcinoma-3 body suspected to be T1b/T2 gallbladder carcinoma-4 (middle
(ischemic demarcation line of S4b). The ischemic demarcation line hepatic vein). The peripheral part of the middle hepatic vein was
(arrowheads) was observed on the liver surface after division of the divided on the transection plane
Glissonian pedicles to S4b. According to this line, liver transection
was performed from left to right, exposing the hilar plate dissected and the root of the cystic duct was exposed
the ischemic demarcation line on the liver surface that and divided. Intraoperative frozen section pathology
of the stump of the cystic duct confirmed the absence
appeared after division of these Glissonian pedicles
and exposure of the right part of the transection line of of tumor invasion. The cystic plate including the cystic
the resected liver (S5+6a of S4b+5+6a) [Figure 7]. The duct, artery, and LNs was attached to the resected
resected liver was extracted in a plastic bag through liver and removed en bloc. The resected liver was
the umbilical port. Abdominal drainage catheters were extracted in a plastic bag through the umbilical port.
routinely placed in the operative area. Abdominal drainage catheters were routinely placed in
the operative area.
GB bed LLR
For GB bed LLR, the operation started with liver Regional LN dissection
parenchymal transection from the left anterior side Additional regional LN dissection was performed after
(in S4) with a 1-cm surgical margin from the GB the liver resection when the tumor was confirmed to
after confirming the locations of the GB bottom in the be T2 GBC. The common bile duct, proper and right
liver bed, GBT, and major vessels by intraoperative hepatic arteries, and portal vein were dissected and
laparoscopic ultrasonography. If needed, adhesions taped [Figure 8]. The surrounding tissue including the
from a previous surgery were dissected before the LNs was resected with the tissues of the common
ultrasonographic examination and transection. The hepatic artery, splenic vein, and posterosuperior
liver parenchymal transection started with use of the surface of the pancreas after performing the Kocher
SonoSurg on the shallow surface of the liver. The maneuver.
BiClamp bipolar forceps, used in a clamp-and-crush
manner, and the CUSA were employed for deep RESULTS
parenchymal transection far from and near the major
vessels, respectively. Small vessels were exposed Conversion, morbidity, and mortality in each
and sealed with energy devices, clipped or ligated, group
and finally divided. Hemostasis of bleeding from the Pathological R0 resection was achieved in all 10
transection surface was accomplished by irrigation patients with GBTs. One patient (10%) developed a
monopolar electric cautery with soft-mode coagulation Clavien-Dindo grade 3 complication (bile leakage) and
or suturing by hand. During the transection, small had a long postoperative LOS (105 days), although no
peripheral branches of G4b, middle hepatic vein, G5, conversions to open procedures or mortality occurred
and G6a were dissected, ligated, and divided. The liver in this group.
transection was performed from left to right and ventral
to dorsal, reaching the right corner of the hilar plate. Among the 79 patients who underwent PR, 2 (2.5%)
underwent conversions to open procedures and 4
When the transection line reached the right corner (5.0%) developed grade 3 postoperative complications
of the hilar plate, the LNs around the bile duct were (postoperative ascites, bile leakage, cholecystitis, and
Hepatoma Research ¦ Volume 3 ¦ August 09, 2017 173