Page 59 - Read Online
P. 59
complete, reliable, and reconstruct a “water tight” barrier The superficial temporal vessels were also palpated and
between the intracranial cavity and the physiologically assessed with Doppler bilaterally to determine the best place
contaminated upper aerodigestive tract. for inset keeping in mind previous scars from operations,
radiation, and/or infections to select the best side for vessel
In 1966, Ketcham et al. first attempted the use of a split dissections. The flap was first de-epithelialized prior to
[5]
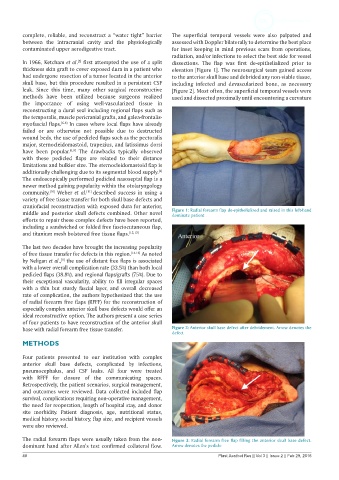
thickness skin graft to cover exposed dura in a patient who elevation [Figure 1]. The neurosurgical team gained access
had undergone resection of a tumor located in the anterior to the anterior skull base and debrided any non-viable tissue,
skull base, but this procedure resulted in a persistent CSF including infected and devascularized bone, as necessary
leak. Since this time, many other surgical reconstructive [Figure 2]. Most often, the superficial temporal vessels were
methods have been utilized because surgeons realized used and dissected proximally until encountering a curvature
the importance of using well-vascularized tissue in
reconstructing a dural seal including regional flaps such as
the temporalis, muscle pericranial grafts, and galea-frontalis-
myofascial flaps. [6-8] In cases where local flaps have already
failed or are otherwise not possible due to destructed
wound beds, the use of pedicled flaps such as the pectoralis
major, sternocleidomastoid, trapezius, and latissimus dorsi
have been popular. [6,9] The drawbacks typically observed
with these pedicled flaps are related to their distance
limitations and bulkier size. The sternocleidomastoid flap is
additionally challenging due to its segmental blood supply.
[4]
The endoscopically performed pedicled nasoseptal flap is a
newer method gaining popularity within the otolaryngology
community. Weber et al. [11] described success in using a
[10]
variety of free tissue transfer for both skull base defects and
craniofacial reconstruction with exposed dura for anterior,
middle and posterior skull defects combined. Other novel Figure 1: Radial forearm flap de-epithelialized and raised in this left-hand
dominate patient
efforts to repair these complex defects have been reported,
including a sandwiched or folded free fasciocutaneous flap,
and titanium mesh bolstered free tissue flaps. [12,13]
The last two decades have brought the increasing popularity
of free tissue transfer for defects in this region. [14-16] As noted
by Neligan et al., the use of distant free flaps is associated
[9]
with a lower overall complication rate (33.5%) than both local
pedicled flaps (38.8%), and regional flaps/grafts (75%). Due to
their exceptional vascularity, ability to fill irregular spaces
with a thin but sturdy fascial layer, and overall decreased
rate of complication, the authors hypothesized that the use
of radial forearm free flaps (RFFF) for the reconstruction of
especially complex anterior skull base defects would offer an
ideal reconstructive option. The authors present a case series
of four patients to have reconstruction of the anterior skull
base with radial forearm free tissue transfer. Figure 2: Anterior skull base defect after debridement. Arrow denotes the
defect
METHODS
Four patients presented to our institution with complex
anterior skull base defects, complicated by infections,
pneumocephalus, and CSF leaks. All four were treated
with RFFF for closure of the communicating spaces.
Retrospectively, the patient scenarios, surgical management,
and outcomes were reviewed. Data collected included flap
survival, complications requiring non-operative management,
the need for reoperation, length of hospital stay, and donor
site morbidity. Patient diagnosis, age, nutritional status,
medical history, social history, flap size, and recipient vessels
were also reviewed.
The radial forearm flaps were usually taken from the non- Figure 3: Radial forearm free flap filling the anterior skull base defect.
dominant hand after Allen’s test confirmed collateral flow. Arrow denotes the pedicle
48 Plast Aesthet Res || Vol 3 || Issue 2 || Feb 29, 2016