Page 356 - Read Online
P. 356
Kanevsky et al. Stretch device for scar therapy
Control scar Sham
0.5× 1× 2×
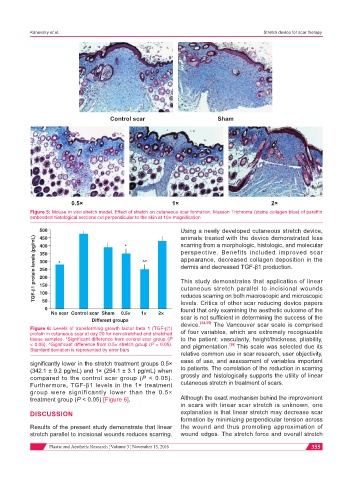
Figure 5: Mouse in vivo stretch model. Effect of stretch on cutaneous scar formation. Masson Trichrome (stains collagen blue) of paraffin
embedded histological sections cut perpendicular to the skin at 10× magnification
500 * Using a newly developed cutaneous stretch device,
animals treated with the device demonstrated less
TGF-β1 protein levels (pg/mL) 350 * ^* perspective. Benefits included improved scar
450
scarring from a morphologic, histologic, and molecular
400
appearance, decreased collagen deposition in the
300
dermis and decreased TGF-β1 production.
250
200
This study demonstrates that application of linear
150
cutaneous stretch parallel to incisional wounds
100
50
levels. Critics of other scar reducing device papers
0 reduces scarring on both macroscopic and microscopic
found that only examining the aesthetic outcome of the
No scar Control scar Sham 0.5× 1× 2×
Different groups scar is not sufficient in determining the success of the
[34,35]
Figure 6: Levels of transforming growth factor beta 1 (TGF-β1) device. The Vancouver scar scale is comprised
protein in cutaneous scar at day 20 for non-stretched and stretched of four variables, which are extremely recognizable
tissue samples. *Significant difference from control scar group (P to the patient: vascularity, height/thickness, pliability,
< 0.05); ^Significant difference from 0.5× stretch group (P < 0.05). and pigmentation. [36] This scale was selected due its
Standard deviation is represented by error bars
relative common use in scar research, user objectivity,
significantly lower in the stretch treatment groups 0.5× ease of use, and assessment of variables important
(342.1 ± 9.2 pg/mL) and 1× (254.1 ± 3.1 pg/mL) when to patients. The correlation of the reduction in scarring
compared to the control scar group (P < 0.05). grossly and histologically supports the utility of linear
Furthermore, TGF-β1 levels in the 1× treatment cutaneous stretch in treatment of scars.
group were significantly lower than the 0.5×
treatment group (P < 0.05) [Figure 6]. Although the exact mechanism behind the improvement
in scars with linear scar stretch is unknown, one
DISCUSSION explanation is that linear stretch may decrease scar
formation by minimizing perpendicular tension across
Results of the present study demonstrate that linear the wound and thus promoting approximation of
stretch parallel to incisional wounds reduces scarring. wound edges. The stretch force and overall stretch
Plastic and Aesthetic Research ¦ Volume 3 ¦ November 15, 2016 355