Page 82 - Read Online
P. 82
Page 6 of 20 Kobylarz et al. Plast Aesthet Res 2023;10:2 https://dx.doi.org/10.20517/2347-9264.2022.38
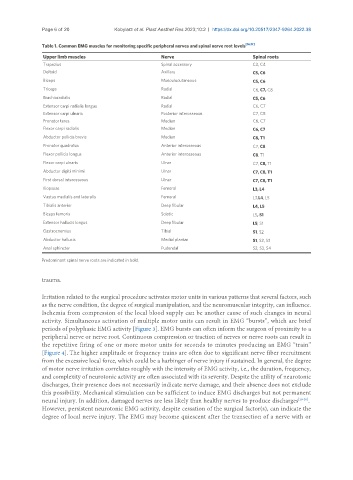
Table 1. Common EMG muscles for monitoring specific peripheral nerves and spinal nerve root levels [16,17]
Upper limb muscles Nerve Spinal roots
Trapezius Spinal accessory C3, C4
Deltoid Axillary C5, C6
Biceps Musculocutaneous C5, C6
Triceps Radial C6, C7, C8
Brachioradialis Radial C5, C6
Extensor carpi radialis longus Radial C6, C7
Extensor carpi ulnaris Posterior interosseous C7, C8
Pronator teres Median C6, C7
Flexor carpi radialis Median C6, C7
Abductor pollicis brevis Median C8, T1
Pronator quadratus Anterior interosseous C7, C8
Flexor pollicis longus Anterior interosseous C8, T1
Flexor carpi ulnaris Ulnar C7, C8, T1
Abductor digiti minimi Ulnar C7, C8, T1
First dorsal interosseous Ulnar C7, C8, T1
Iliopsoas Femoral L3, L4
Vastus medialis and lateralis Femoral L3,L4, L5
Tibialis anterior Deep fibular L4, L5
Biceps femoris Sciatic L5, S1
Extensor hallucis longus Deep fibular L5, S1
Gastrocnemius Tibial S1, S2
Abductor hallucis Medial plantar S1, S2, S3
Anal sphincter Pudendal S2, S3, S4
Predominant spinal nerve roots are indicated in bold.
trauma.
Irritation related to the surgical procedure activates motor units in various patterns that several factors, such
as the nerve condition, the degree of surgical manipulation, and the neuromuscular integrity, can influence.
Ischemia from compression of the local blood supply can be another cause of such changes in neural
activity. Simultaneous activation of multiple motor units can result in EMG “bursts”, which are brief
periods of polyphasic EMG activity [Figure 3]. EMG bursts can often inform the surgeon of proximity to a
peripheral nerve or nerve root. Continuous compression or traction of nerves or nerve roots can result in
the repetitive firing of one or more motor units for seconds to minutes producing an EMG “train”
[Figure 4]. The higher amplitude or frequency trains are often due to significant nerve fiber recruitment
from the excessive local force, which could be a harbinger of nerve injury if sustained. In general, the degree
of motor nerve irritation correlates roughly with the intensity of EMG activity, i.e., the duration, frequency,
and complexity of neurotonic activity are often associated with its severity. Despite the utility of neurotonic
discharges, their presence does not necessarily indicate nerve damage, and their absence does not exclude
this possibility. Mechanical stimulation can be sufficient to induce EMG discharges but not permanent
neural injury. In addition, damaged nerves are less likely than healthy nerves to produce discharges [18-20] .
However, persistent neurotonic EMG activity, despite cessation of the surgical factor(s), can indicate the
degree of local nerve injury. The EMG may become quiescent after the transection of a nerve with or