Page 30 - Read Online
P. 30
Preto et al. Plast Aesthet Res. 2025;12:28 https://dx.doi.org/10.20517/2347-9264.2025.26 Page 11 of 17
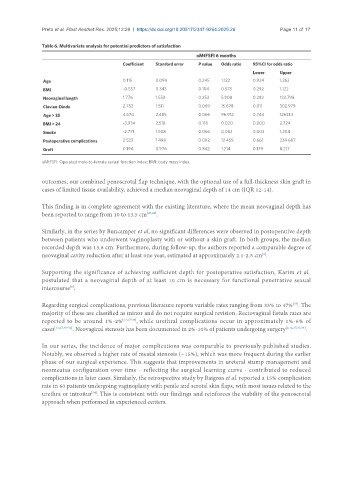
Table 6. Multivariate analysis for potential predictors of satisfaction
oMtFSFI 6 months
Coefficient Standard error P value Odds ratio 95%CI for odds ratio
Lower Upper
Age 0.115 0.099 0.245 1.122 0.924 1.363
BMI -0.557 0.343 0.104 0.573 0.292 1.122
Neovaginal length 1.776 1.552 0.253 5.908 0.282 123.798
Clavien-Dindo 2.752 1.511 0.069 15.678 0.811 302.979
Age > 35 4.574 2.485 0.066 96.912 0.744 12631.3
BMI > 24 -3.934 2.518 0.118 0.020 0.000 2.724
Smoke -2.771 1.508 0.066 0.063 0.003 1.204
Postoperative complications 2.522 1.498 0.092 12.459 0.661 234.687
Graft 0.194 0.976 0.842 1.214 0.179 8.217
oMtFSFI: Operated male-to-female sexual function index; BMI: body mass index.
outcomes, our combined penoscrotal flap technique, with the optional use of a full-thickness skin graft in
cases of limited tissue availability, achieved a median neovaginal depth of 14 cm (IQR 12-14).
This finding is in complete agreement with the existing literature, where the mean neovaginal depth has
been reported to range from 10 to 13.5 cm [27,28] .
Similarly, in the series by Buncamper et al, no significant differences were observed in postoperative depth
between patients who underwent vaginoplasty with or without a skin graft. In both groups, the median
recorded depth was 13.8 cm. Furthermore, during follow-up, the authors reported a comparable degree of
neovaginal cavity reduction after at least one year, estimated at approximately 2.1-2.5 cm .
[6]
Supporting the significance of achieving sufficient depth for postoperative satisfaction, Karim et al.
postulated that a neovaginal depth of at least 10 cm is necessary for functional penetrative sexual
intercourse .
[5]
Regarding surgical complications, previous literature reports variable rates ranging from 33% to 47% . The
[29]
majority of these are classified as minor and do not require surgical revision. Rectovaginal fistula rates are
reported to be around 1%-2% [12,27-29] , while urethral complications occur in approximately 1%-6% of
cases [12,27,30-32] . Neovaginal stenosis has been documented in 2%-10% of patients undergoing surgery [2,12,27,31,33] .
In our series, the incidence of major complications was comparable to previously published studies.
Notably, we observed a higher rate of meatal stenosis (~15%), which was more frequent during the earlier
phase of our surgical experience. This suggests that improvements in ureteral stump management and
neomeatus configuration over time - reflecting the surgical learning curve - contributed to reduced
complications in later cases. Similarly, the retrospective study by Raigosa et al. reported a 15% complication
rate in 60 patients undergoing vaginoplasty with penile and scrotal skin flaps, with most issues related to the
urethra or introitus . This is consistent with our findings and reinforces the viability of the penoscrotal
[34]
approach when performed in experienced centers.