Page 140 - Read Online
P. 140
Alam et al. Neuroimmunol Neuroinflammation 2018;5:21 I http://dx.doi.org/10.20517/2347-8659.2017.64 Page 5 of 10
Gender No. of patients Percentage
Male 3 30.0%
Female 7 70.0%
Total 10 100.0%
Age group (in years) No. of patients Percentage
21-30 1 10.0%
31-40 1 10.0%
41-50 7 70.0%
51-60 1 10.0%
Total 10 100.0% Figure 2. Following craniotomy shows removal of anterior clinoid process and unroofing of optic foramen
Mean age 45 ± 13.12 years
A B
Extent of tumor removal No. of patient Percentage
Gross total 5 50.0%
Near total 5 50.0%
Total 10 100.0%
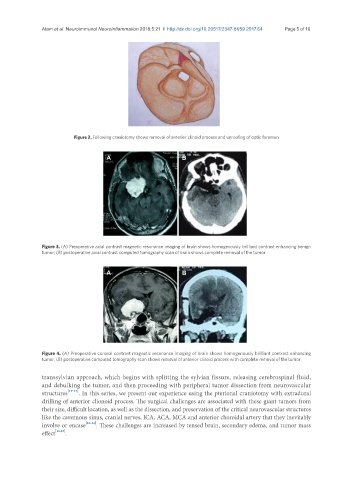
Figure 3. (A) Preoperative axial contrast magnetic resonance imaging of brain shows homogenously brilliant contrast enhancing benign
tumor; (B) postoperative axial contrast computed tomography scan of brain shows complete removal of the tumor
Functional outcome No. of patients Percentage A B
Improved 7 70.0%
Static 2 20.0%
Deteriorated 1 10.0%
Total 10 100.0%
Figure 4. (A) Preoperative coronal contrast magnetic resonance imaging of brain shows homogenously brilliant contrast enhancing
tumor; (B) postoperative computed tomography scan shows removal of anterior clinoid process with complete removal of the tumor
transsylvian approach, which begins with splitting the sylvian fissure, releasing cerebrospinal fluid,
and debulking the tumor, and then proceeding with peripheral tumor dissection from neurovascular
structures [19-21] . In this series, we present our experience using the pterional craniotomy with extradural
drilling of anterior clionoid process. The surgical challenges are associated with these giant tumors from
their size, difficult location, as well as the dissection, and preservation of the critical neurovascular structures
like the cavernous sinus, cranial nerves, ICA, ACA, MCA and anterior choroidal artery that they inevitably
involve or encase [22-24] . These challenges are increased by tensed brain, secondary edema, and tumor mass
effect [18,25] .