Page 126 - Read Online
P. 126
Nwabuobi et al. Thymoma associated panencephalitis
seizures. The target antigen when it manifests in hyperexcitability over the right temporal region and
[3]
thymomas is largely unknown, however, some cases frequent focal seizures and he was empirically treated
have reported antibodies to α-amino-3-hydroxy-5- with IV acyclovir, lacosamide and levetiracetam.
methylisoxazole-4-proprionic acid receptor, leucine- Cerebral spinal fluid (CSF) analysis revealed protein
rich glioma inactivated 1 protein (LGI1), contactin of 0.51 g/L, glucose of 3.5 mmol/L, 3 × 10 /L red
-6
associated protein 2 (Caspr2), and glutamic acid blood cells and 9 × 10 /L white blood cells (76%
-6
decarboxylase (GAD). A new entity has been lymphocytes, 18% monocytes, 6% neutrophils). CSF
[4]
described in a few cases of paraneoplastic encephalitis and serum studies were also positive for neuronal
associated with thymomas, with lesions extending antibodies to GAD [3.93 nmol/L in the CSF (normal <
beyond the mesial temporal lobe structures. 0.02 nmol/L), > 250.0 kIU/L in the serum (reference
range 0-5 kIU/L)], VGKC-complex antibodies [159 pmol/L
CASE REPORT in the CSF (reference range 0-31 pmol/L), 98 pmol/L
in the serum (reference range 0-31 pmol/L)], CRMP5
A 35-year-old man presented with a 2-week history (reflex titer < 1:240; positive western blot), and AchR
of seizures, poor appetite, generalized headaches [binding antibody 17.5 nmol/L in the CSF (normal
and nausea. Neurologic assessment revealed poor < 0.02 nmol/L), and 142.8 nmol/L in the serum
attention, orientation and memory loss, without (reference range 0.0-0.4 nmol/L)]. Additionally, serum
clinical seizures. Computed tomography head showed studies revealed presence of systemic antibodies to
multiple cortical hypodensities, prompting an magnetic thyroperoxidase (37.8 kIU/L, reference range 0-5.5 kIU/L),
resonance imaging (MRI) brain, which revealed thyroglobulin (372.2 kIU/L, reference range 0-5 kIU/L),
multiple foci of cortical hyperintensity involving the Ro/SSA (6.8 AI, reference range < 1 AI), and an ANA
medial left frontal cortex, the right dorsal aspect of the titer of 80 (reference range 0-40) with a nucleolar
insula and adjacent right temporal cortex as well as the pattern. A paraneoplastic syndrome was suspected,
posterior left temporal cortical medullary junction and and full body imaging revealed a large multilobulated
the medial posterior left temporal cortex and lateral right anterior mediastinal mass, interfacing multiple
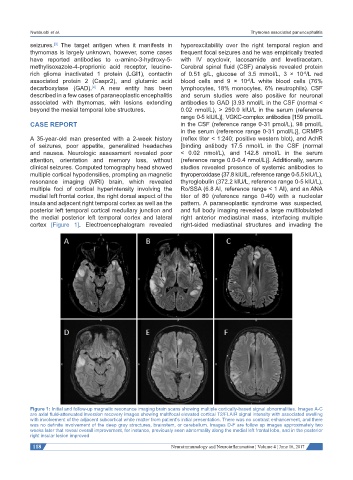
cortex [Figure 1]. Electroencephalogram revealed right-sided mediastinal structures and invading the
Figure 1: Initial and follow-up magnetic resonance imaging brain scans showing multiple cortically-based signal abnormalities. Images A-C
are axial fluid-attenuated inversion recovery images showing multifocal elevated cortical T2/FLAIR signal intensity with associated swelling
with involvement of the adjacent subcortical white matter from patient’s initial presentation. There was no contrast enhancement, and there
was no definite involvement of the deep gray structures, brainstem, or cerebellum. Images D-F are follow up images approximately two
weeks later that reveal overall improvement, for instance, previously seen abnormality along the medial left frontal lobe, and in the posterior
right insular lesion improved
118 Neuroimmunology and Neuroinflammation ¦ Volume 4 ¦ June 16, 2017