Page 253 - Read Online
P. 253
Agarwal et al. CVT in UC relapse
CVT is a uncommon type of cerebrovascular disease signal intensity was visualized in the Torcula and the
that accounts for 0.5% of all strokes. It usually right sided transverse sinus. Also a note was made of
[5]
presents as headache, seizures, focal neurological a large left sided fronto-temporo-parietal and occipital
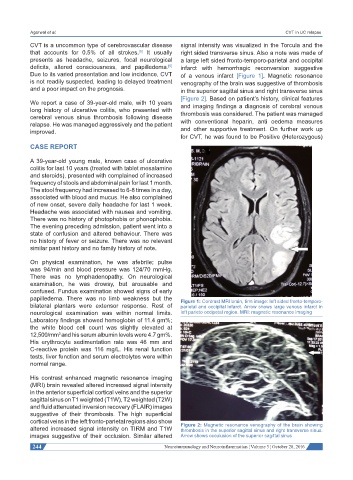
deficits, altered consciousness, and papilledema. infarct with hemorrhagic reconversion suggestive
[6]
Due to its varied presentation and low incidence, CVT of a venous infarct [Figure 1]. Magnetic resonance
is not readily suspected, leading to delayed treatment venography of the brain was suggestive of thrombosis
and a poor impact on the prognosis. in the superior sagittal sinus and right transverse sinus
[Figure 2]. Based on patient’s history, clinical features
We report a case of 39-year-old male, with 10 years and imaging findings a diagnosis of cerebral venous
long history of ulcerative colitis, who presented with thrombosis was considered. The patient was managed
cerebral venous sinus thrombosis following disease
relapse. He was managed aggressively and the patient with conventional heparin, anti oedema measures
improved. and other supportive treatment. On further work up
for CVT, he was found to be Positive (Heterozygous)
CASE REPORT
A 39-year-old young male, known case of ulcerative
colitis for last 10 years (treated with tablet mesalamine
and steroids), presented with complained of increased
frequency of stools and abdominal pain for last 1 month.
The stool frequency had increased to 6-8 times in a day,
associated with blood and mucus. He also complained
of new onset, severe daily headache for last 1 week.
Headache was associated with nausea and vomiting.
There was no history of photophobia or phonophobia.
The evening preceding admission, patient went into a
state of confusion and altered behaviour. There was
no history of fever or seizure. There was no relevant
similar past history and no family history of note.
On physical examination, he was afebrile; pulse
was 94/min and blood pressure was 124/70 mmHg.
There was no lymphadenopathy. On neurological
examination, he was drowsy, but arousable and
confused. Fundus examination showed signs of early
papilledema. There was no limb weakness but the Figure 1: Contrast MRI brain, tirm image: left sided fronto-temporo-
bilateral plantars were extensor response. Rest of parietal and occipital infarct. Arrow shows large venous infarct in
neurological examination was within normal limits. left parieto occipetal region. MRI: magnetic resonance imaging
Laboratory findings showed hemoglobin of 11.4 gm%;
the white blood cell count was slightly elevated at
12,500/mm and his serum albumin levels were 4.7 gm%.
3
His erythrocyte sedimentation rate was 46 mm and
C-reactive protein was 116 mg/L. His renal function
tests, liver function and serum electrolytes were within
normal range.
His contrast enhanced magnetic resonance imaging
(MRI) brain revealed altered increased signal intensity
in the anterior superficial cortical veins and the superior
sagittal sinus on T1 weighted (T1W), T2 weighted (T2W)
and fluid attenuated inversion recovery (FLAIR) images
suggestive of their thrombosis. The high superficial
cortical veins in the left fronto-parietal regions also show Figure 2: Magnetic resonance venography of the brain showing
altered increased signal intensity on TIRM and T1W thrombosis in the superior sagittal sinus and right transverse sinus.
images suggestive of their occlusion. Similar altered Arrow shows occulusion of the superior sagittal sinus
244 Neuroimmunology and Neuroinflammation ¦ Volume 3 ¦ October 28, 2016