Page 230 - Read Online
P. 230
Menon et al. Pediatric anti-GAD antibody mediated encephalitis
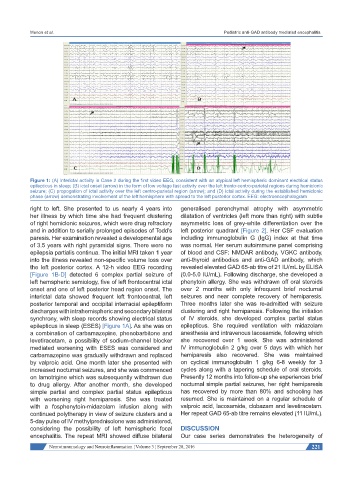
Figure 1: (A) Interictal activity in Case 2 during the first video EEG, consistent with an atypical left hemispheric dominant electrical status
epilepticus in sleep; (B) ictal onset (arrow) in the form of low voltage fast activity over the left fronto-centro-parietal regions during hemiclonic
seizure; (C) propogation of ictal activity over the left centro-parietal region (arrow); and (D) ictal activity during the established hemiclonic
phase (arrow) demonstrating involvement of the left hemisphere with spread to the left posterior cortex. EEG: electroencephalogram
right to left. She presented to us nearly 4 years into generalised parenchymal atrophy with asymmetric
her illness by which time she had frequent clustering dilatation of ventricles (left more than right) with subtle
of right hemiclonic seizures, which were drug refractory asymmetric loss of grey-white differentiation over the
and in addition to serially prolonged episodes of Todd’s left posterior quadrant [Figure 2]. Her CSF evaluation
paresis. Her examination revealed a developmental age including immunoglobulin G (IgG) index at that time
of 3.5 years with right pyramidal signs. There were no was normal. Her serum autoimmune panel comprising
epilepsia partialis continua. The initial MRI taken 1 year of blood and CSF: NMDAR antibody, VGKC antibody,
into the illness revealed non-specific volume loss over anti-thyroid antibodies and anti-GAD antibody, which
the left posterior cortex. A 12-h video EEG recording revealed elevated GAD 65-ab titre of 21 IU/mL by ELISA
[Figure 1B-D] detected 6 complex partial seizure of (0.0-5.0 IU/mL). Following discharge, she developed a
left hemspheric semiology, five of left frontocentral ictal phenytoin allergy. She was withdrawn off oral steroids
onset and one of left posterior head region onset. The over 2 months with only infrequent brief nocturnal
interictal data showed frequent left frontocentral, left seizures and near complete recovery of hemiparesis.
posterior temporal and occipital interracial epileptiform Three months later she was re-admitted with seizure
discharges with intrahemispheric and secondary bilateral clustering and right hemiparesis. Following the initiation
synchrony, with sleep records showing electrical status of IV steroids, she developed complex partial status
epilepticus in sleep (ESES) [Figure 1A]. As she was on epilepticus. She required ventilation with midazolam
a combination of carbamazepine, phenobarbitone and anesthesia and intravenous lacosamide, following which
levetiracetam, a possibility of sodium-channel blocker she recovered over 1 week. She was administered
mediated worsening with ESES was considered and IV immunoglobulin 2 g/kg over 5 days with which her
carbamazepine was gradually withdrawn and replaced hemiparesis also recovered. She was maintained
by valproic acid. One month later she presented with on cyclical immunoglobulin 1 g/kg 6-8 weekly for 3
increased nocturnal seizures, and she was commenced cycles along with a tapering schedule of oral steroids.
on lamotrigine which was subsequently withdrawn due Presently 12 months into follow-up she experiences brief
to drug allergy. After another month, she developed nocturnal simple partial seizures, her right hemiparesis
simple partial and complex partial status epilepticus has recovered by more than 80% and schooling has
with worsening right hemiparesis. She was treated resumed. She is maintained on a regular schedule of
with a fosphenytoin-midazolam infusion along with valproic acid, lacosamide, clobazam and levetiracetam.
continued polytherapy in view of seizure clusters and a Her repeat GAD 65-ab titre remains elevated (11 IU/mL).
5-day pulse of IV methylprednisolone was administered,
considering the possibility of left hemispheric focal DISCUSSION
encephalitis. The repeat MRI showed diffuse bilateral Our case series demonstrates the heterogeneity of
Neuroimmunology and Neuroinflammation ¦ Volume 3 ¦ September 28, 2016 221