Page 145 - Read Online
P. 145
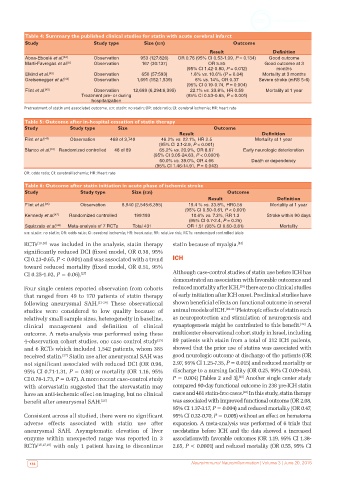
Table 4: Summary the published clinical studies for statin with acute cerebral infarct
Study Study type Size (s:n) Outcome
Result Definition
Aboa-Eboulé et al. [42] Observation 953 (127:826) OR 0.76 (95% CI 0.53-1.09, P = 0.134) Good outcome
Marti-Favregas et al. [8] Observation 167 (30:137) OR 5.55 Good outcome at 3
(95% CI 1.42-0.80, P = 0.012) months
Elkind et al. [43] Observation 650 (57:593) 1.8% vs. 10.6% (P = 0.04) Mortality at 3 months
Greisenegger et al. [44] Observation 1,691 (152:1,539) 6% vs. 14%, OR 0.37 Severe stroke (mRS 5-6)
(95% CI 0.19-0.74, P = 0.004)
Flint et al. [45] Observation 12,689 (6,294:6,395) 22.1% vs. 33.8%, HR 0.59 Mortality at 1 year
Treatment pre- or during (95% CI 0.53-0.65, P < 0.001)
hospitalization
Pretreatment of statin and associated outcome. s:n: statin: no statin; OR: odds ratio; CI: cerebral ischemia; HR: heart rate
Table 5: Outcome after in-hospital cessation of statin therapy
Study Study type Size Outcome
Result Definition
Flint et al. [45] Observation 468 of 3,749 46.2% vs. 22.1%, HR 2.5 Mortality at 1 year
(95% CI 2.1-2.9, P < 0.001)
Blanco et al. [46] Randomized controlled 46 of 89 65.2% vs. 20.9%, OR 8.67 Early neurologic deterioration
(95% CI 3.05-24.63, P < 0.0001)
60.0% vs. 39.0%, OR 4.66 Death or dependency
(95% CI 1.46-14.91, P = 0.043)
OR: odds ratio; CI: cerebral ischemia; HR: Heart rate
Table 6: Outcome after statin initiation in acute phase of ischemic stroke
Study Study type Size (s:n) Outcome
Result Definition
Flint et al. [45] Observation 8,940 (2,545:6,395) 19.4 % vs. 33.8%, HR0.55 Mortality at 1 year
(95% CI 0.50-0.61, P < 0.001)
Kennedy et al. [47] Randomized controlled 199:193 10.6% vs. 7.3%, RR 1.3 Stroke within 90 days
(95% CI 0.7-2.4, P = 0.25)
Squizzato et al. [48] Meta-analysis of 7 RCTs Total 431 OR 1.51 (95% CI 0.60-3.81) Mortality
s:n: statin: no statin; OR: odds ratio; CI: cerebral ischemia; HR: heart rate; RR: relative risk; RCTs: randomized controlled trials
RCTs [19,20] was included in the analysis, statin therapy statin because of myalgia. [18]
significantly reduced DCI (fixed model, OR 0.38, 95%
CI 0.23-0.65, P < 0.001) and was associated with a trend ICH
toward reduced mortality (fixed model, OR 0.51, 95%
CI 0.25-1.02, P = 0.06). [27] Although case-control studies of statin use before ICH has
demonstrated an association with favorable outcomes and
[28]
Four single centers reported observation from cohorts reduced mortality after ICH, there are no clinical studies
that ranged from 49 to 170 patients of statin therapy of early initiation after ICH onset. Preclinical studies have
following aneurysmal SAH. [21-24] These observational shown beneficial effects on functional outcome in several
studies were considered to low quality because of animal models of ICH. [29-31] Pleiotropic effects of statin such
relatively small sample sizes, heterogeneity in baseline, as neuroprotection and stimulation of neurogenesis and
[32]
clinical management and definition of clinical synaptogenesis might be contributed to this benefit. A
outcome. A meta-analysis was performed using these multicenter observational cohort study in Israel, including
4-observation cohort studies, one case control study 89 patients with statin from a total of 312 ICH patients,
[25]
and 6 RCTs which included 1,542 patients, whom 385 showed that the prior use of statins was associated with
[27]
received statin. Statin use after aneurysmal SAH was good neurologic outcome at discharge of the patients (OR
not significant associated with reduced DCI (OR 0.96, 2.97, 95% CI 1.25-7.35, P = 0.015) and reduced mortality or
95% CI 0.71-1.31, P = 0.80) or mortality (OR 1.16, 95% discharge to a nursing facility (OR 0.25, 95% CI 0.09-0.63,
[33]
CI 0.78-1.73, P = 0.47). A more recent case-control study P = 0.004) [Tables 2 and 3]. Another single center study
with atorvastatin suggested that the atorvastatin may compared 90-day functional outcome in 238 pre-ICH statin
[28]
have an anti-ischemic effect on imaging, but no clinical cases and 461 statin-free cases. In this study, statin therapy
benefit after aneurysmal SAH. [26] was associated with improved functional outcome (OR 2.08,
95% CI 1.37-3.17, P = 0.004) and reduced mortality (OR 0.47,
Consistent across all studied, there were no significant 95% CI 0.32-0.70, P = 0.005) without an effect on hematoma
adverse effects associated with statin use after expansion. A meta-analysis was performed of 6 trials that
aneurysmal SAH. Asymptomatic elevation of liver usedstatins before ICH and the data showed a increased
enzyme within unexpected range was reported in 3 associationwith favorable outcomes (OR 1.19, 95% CI 1.38-
RCTs [15,17,18] with only 1 patient having to discontinue 2.65, P < 0.0001) and reduced mortality (OR 0.55, 95% CI
136 Neuroimmunol Neuroinflammation | Volume 3 | June 20, 2016