Page 114 - Read Online
P. 114
veins in the dural border cell layer, causing them to EBP is a feasible and efficient treatment for SIH with
rupture and leading to subdural hematoma; (2) the CSF leak in the cervical area, subdural hematoma and
loss of CSF volume reduces absorption of CSF into the CVT.
cerebral venous sinuses, resulting in increased blood
[5]
viscosity in the venous compartment, which could CASE REPORT
contribute to dural sinus thrombosis in patients with
risk factors for thrombosis. The general consensus A 48 years old Indian male presented with headache
is that CVT should be treated with heparin, since a and neck pain of 1 month duration. The patient had
meta-analysis concluded that this treatment is safe severe occipital headache with visual analogue score
and is associated with a clinical trend (not statistically of 9. The headache worsened in the upright position
significant) of reduction in the risk of death and and was completely relieved after lying down. The
dependency. Thus, most of the reported SIH patients patient was otherwise normal, without any significant
with CVT have been treated with anticoagulation so past clinical history.
far along with bed rest, hydration and epidural blood On examination, the patient was conscious, oriented
patches (EBP) [Table 2]. [6-14] On the other hand, cases of and afebrile, with a pulse rate of 82 beats per minute
large subdural hemorrhage require surgical drainage and blood pressure of 130/80 mmHg. Eye movements
and treatment of the underlying cause of SIH. Most were normal in all directions and there was no sign
SIH patients without other complications recover of nystagmus. Both pupils were equal and reactive to
after bed rest with foot end elevation, hydration and light. Cranial nerve and fundus examinations were
steroid therapy. Nevertheless, the mainstay of SIH also normal and no motor weakness or sensory loss
treatment is the application of EBP at the CSF-leak was present. Flexor plantar response was positive and
site (injection of 10-20 mL of autologous blood into bilateral. No signs of meningeal irritation nor focal
the spinal epidural space). [15] Relief of symptoms, neurological deficits were found.
particularly orthostatic headache, is often dramatic
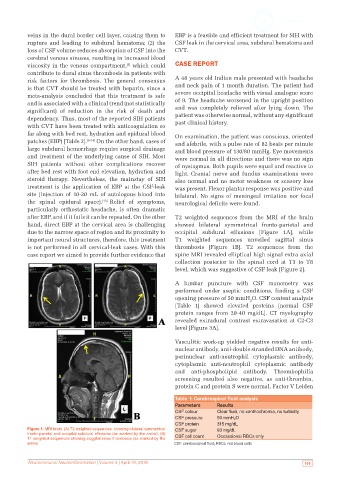
after EBP, and if it fails it can be repeated. On the other T2 weighted sequences from the MRI of the brain
hand, direct EBP at the cervical area is challenging showed bilateral symmetrical fronto-parietal and
due to the narrow space of region and its proximity to occipital subdural effusions [Figure 1A], while
important neural structures, therefore, this treatment T1 weighted sequences unveiled sagittal sinus
is not performed in all cervical-leak cases. With this thrombosis [Figure 1B]. T2 sequences from the
case report we aimed to provide further evidence that spine MRI revealed elliptical high signal extra axial
collection posterior to the spinal cord at T3 to T8
level, which was suggestive of CSF leak [Figure 2].
A lumbar puncture with CSF manometry was
performed under aseptic conditions, finding a CSF
opening pressure of 50 mmH O. CSF content analysis
2
[Table 1] showed elevated proteins [normal CSF
protein ranges from 20-40 mg/dL]. CT myelography
revealed extradural contrast extravasation at C2-C3
level [Figure 3A].
Vasculitic work-up yielded negative results for anti-
nuclear antibody, anti-double stranded DNA antibody,
perinuclear anti-neutrophil cytoplasmic antibody,
cytoplasmic anti-neutrophil cytoplasmic antibody
and anti-phospholipid antibody. Thrombophilia
screening resulted also negative, as anti-thrombin,
protein C and protein S were normal. Factor V Leiden
Table 1: Cerebrospinal fluid analysis
Parameters Results
CSF colour Clear fluid, no xanthochromia, no turbidity
CSF pressure 50 mmH 2 O
CSF protein 315 mg/dL
Figure 1: MRI brain. (A) T2 weighted sequences showing bilateral symmetrical CSF sugar 93 mg/dL
fronto-parietal and occipital subdural effusions (as marked by the arrow); (B) CSF cell count Occassional RBCs only
T1 weighted sequences showing saggital sinus thrombosis (as marked by the
arrow) CSF: cerebrospinal fluid; RBCs: red blood cells
Neuroimmunol Neuroinflammation | Volume 3 | April 19, 2016 105