Page 296 - Read Online
P. 296
and glucose levels within normal limits. A presumptive obstructive hydrocephalus secondary to a trapped
diagnosis of idiopathic hydrocephalus was made. ventricle with a left‑to‑right midline shift, so a left
A right frontal external ventricular drain was placed frontal ventriculoperitoneal shunt was placed.
followed by right frontal ventriculoperitoneal shunt Although postoperative MRI revealed decreased
placement. A postoperative head CT revealed a hydrocephalus, the third and fourth ventricles
collapsed right lateral ventricle and unchanged left remained prominent. No postcontrast enhancement
lateral, third, and fourth ventricles. Due to symptomatic was seen [Figure 1a and b].
improvement, the unresolved hydrocephalus was
followed without further intervention. Other than one shunt revision, she remained relatively
stable for 3 years after which she presented to the
Five months later, the patient presented to the outside hospital with unsteadiness, double vision,
outside hospital with a headache, nausea, vomiting, and left leg weakness. Head CT revealed collapsed
ataxia, dizziness, and blurred vision. Other than an lateral and third ventricles and a persistent dilatation
opening pressure of 25 cm of H O and glucose of of the fourth ventricle, which prompted placement of
2
97 mg/dL, CSF analysis was within normal limits. a ventriculoperitoneal shunt in the fourth ventricle.
Angiotensin‑converting enzyme (ACE) levels She was discharged, but her condition continued
were not tested. Head CT revealed left unilateral to deteriorate, possibly due to over‑shunting or disease
progression and she was readmitted after 2 weeks. At
this point, she transferred her care to our institution.
Table 1: Signs and symptoms of neurosarcoidosis
Sign or symptom Percent affected (%) References
Cranial neuropathy 52‑73 [3,4-6] Upon arrival, her neurological exam demonstrated
Aseptic meningitis 7-24 [3,4-6] direction‑changing nystagmus, asymmetric proximal
Peripheral neuropathy 6-24 [3-6] lower extremity weakness (iliopsoas right 3/5, left 2/5),
Cognitive impairment 2‑27 [4,5] and ataxia on finger‑nose‑finger and heel‑shin testing.
Seizures 2‑20 [4-6]
Myopathy 9‑12 [3,6] There were no sensory deficits, and the patient did not
CNS space occupying lesion 2‑11 [4-6] complain of fecal or urinary incontinence. Head CT
HPA axis dysfunction 2‑11 [4-6] demonstrated bilateral frontal and right suboccipital
Hydrocephalus 4-9 [3,6]
Paresthesia 43 [4] approach ventricular catheters and a decompressed
Headache 37 [4] ventricular system. Hypo‑density, suggestive of
Weakness 33 [4] edema, in the cerebellum prompted treatment with
Ataxia 24 [6]
Myelopathy 21 [4] Decadron. MRI revealed sulcal enhancement bilaterally
Encephalopathy 11 [6] along the frontal lobes and internal auditory canals
Hemiparesis 7 [4] that suggested leptomeningeal disease [Figure 1c
Guillain‑Barré syndrome 5 [5]
Radiculopathy 3 [4] and d]. MRI of the spine revealed diffuse nodular
CNS: central nervous system; HPA: hypothalamic pituitary adrenal leptomeningeal enhancement throughout the spinal
a b c d e f
g h i
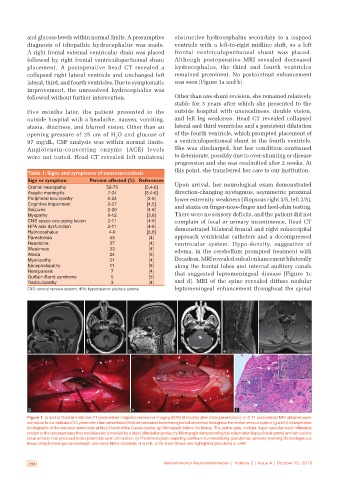
Figure 1: (a and b) Outside institution T1 postcontrast magnetic resonance imaging (MRI) (5 months after initial presentation); (c‑f) T1 postcontrast MRI obtained upon
admission to our institution (3.5 years after initial presentation) that demonstrates leptomeningeal enhancement throughout the central nervous system; (g and h) Intraoperative
photographs of the exposed nerve roots at the L3 level of the Cauda equina; (g) Micrograph before the biopsy. The yellow‑gray, nodular, hyper‑vascular lesion intimately
related to the leptomeninges that was biopsied is marked by a black stimulation probe; (h) Micrograph demonstrating the lesion after biopsy (black arrow) and two lesions
(blue arrows) that produced motor potentials upon stimulation; (i) Photomicrograph depicting confluent nonnecrotizing granulomas (arrows) involving fibrocollagenous
tissue of leptomeninges (arrowhead), and nerve fibers (asterisk); H and E, ×100. Inset shows one highlighted granuloma at ×400
288 Neuroimmunol Neuroinflammation | Volume 2 | Issue 4 | October 15, 2015 Neuroimmunol Neuroinflammation | Volume 2 | Issue 4 | October 15, 2015 289