Page 804 - Read Online
P. 804
Page 4 of 11 Tredway et al. Mini-invasive Surg 2020;4:78 I http://dx.doi.org/10.20517/2574-1225.2020.77
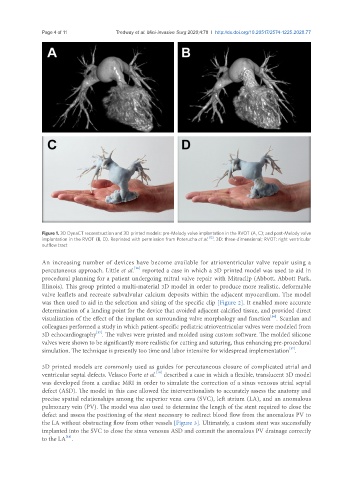
Figure 1. 3D DynaCT reconstruction and 3D printed models: pre-Melody valve implantation in the RVOT (A, C); and post-Melody valve
implantation in the RVOT (B, D). Reprinted with permission from Poterucha et al. [12] . 3D: three-dimensional; RVOT: right ventricular
outflow tract
An increasing number of devices have become available for atrioventricular valve repair using a
[16]
percutaneous approach. Little et al. reported a case in which a 3D printed model was used to aid in
procedural planning for a patient undergoing mitral valve repair with Mitraclip (Abbott, Abbott Park,
Illinois). This group printed a multi-material 3D model in order to produce more realistic, deformable
valve leaflets and recreate subvalvular calcium deposits within the adjacent myocardium. The model
was then used to aid in the selection and sizing of the specific clip [Figure 2]. It enabled more accurate
determination of a landing point for the device that avoided adjacent calcified tissue, and provided direct
[16]
visualization of the effect of the implant on surrounding valve morphology and function . Scanlan and
colleagues performed a study in which patient-specific pediatric atrioventricular valves were modeled from
3D echocardiography . The valves were printed and molded using custom software. The molded silicone
[17]
valves were shown to be significantly more realistic for cutting and suturing, thus enhancing pre-procedural
[17]
simulation. The technique is presently too time and labor intensive for widespread implementation .
3D printed models are commonly used as guides for percutaneous closure of complicated atrial and
[18]
ventricular septal defects. Velasco Forte et al. described a case in which a flexible, translucent 3D model
was developed from a cardiac MRI in order to simulate the correction of a sinus venosus atrial septal
defect (ASD). The model in this case allowed the interventionalists to accurately assess the anatomy and
precise spatial relationships among the superior vena cava (SVC), left atrium (LA), and an anomalous
pulmonary vein (PV). The model was also used to determine the length of the stent required to close the
defect and assess the positioning of the stent necessary to redirect blood flow from the anomalous PV to
the LA without obstructing flow from other vessels [Figure 3]. Ultimately, a custom stent was successfully
implanted into the SVC to close the sinus venosus ASD and commit the anomalous PV drainage correctly
[18]
to the LA .