Page 808 - Read Online
P. 808
Page 8 of 11 Tredway et al. Mini-invasive Surg 2020;4:78 I http://dx.doi.org/10.20517/2574-1225.2020.77
A B
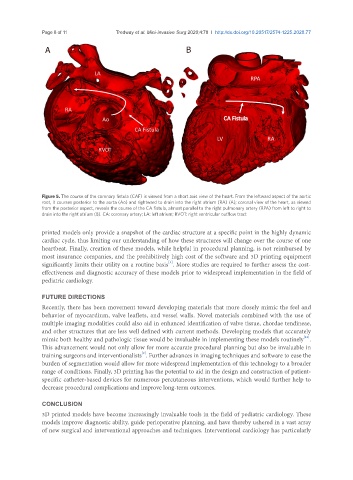
Figure 5. The course of the coronary fistula (CAF) is viewed from a short axis view of the heart. From the leftward aspect of the aortic
root, it courses posterior to the aorta (Ao) and rightward to drain into the right atrium (RA) (A); coronal view of the heart, as viewed
from the posterior aspect, reveals the course of the CA fistula, almost parallel to the right pulmonary artery (RPA) from left to right to
drain into the right atrium (B). CA: coronary artery; LA: left atrium; RVOT: right ventricular outflow tract
printed models only provide a snapshot of the cardiac structure at a specific point in the highly dynamic
cardiac cycle, thus limiting our understanding of how these structures will change over the course of one
heartbeat. Finally, creation of these models, while helpful in procedural planning, is not reimbursed by
most insurance companies, and the prohibitively high cost of the software and 3D printing equipment
[1]
significantly limits their utility on a routine basis . More studies are required to further assess the cost-
effectiveness and diagnostic accuracy of these models prior to widespread implementation in the field of
pediatric cardiology.
FUTURE DIRECTIONS
Recently, there has been movement toward developing materials that more closely mimic the feel and
behavior of myocardium, valve leaflets, and vessel walls. Novel materials combined with the use of
multiple imaging modalities could also aid in enhanced identification of valve tissue, chordae tendineae,
and other structures that are less well defined with current methods. Developing models that accurately
[15]
mimic both healthy and pathologic tissue would be invaluable in implementing these models routinely .
This advancement would not only allow for more accurate procedural planning but also be invaluable in
[2]
training surgeons and interventionalists . Further advances in imaging techniques and software to ease the
burden of segmentation would allow for more widespread implementation of this technology to a broader
range of conditions. Finally, 3D printing has the potential to aid in the design and construction of patient-
specific catheter-based devices for numerous percutaneous interventions, which would further help to
decrease procedural complications and improve long-term outcomes.
CONCLUSION
3D printed models have become increasingly invaluable tools in the field of pediatric cardiology. These
models improve diagnostic ability, guide perioperative planning, and have thereby ushered in a vast array
of new surgical and interventional approaches and techniques. Interventional cardiology has particularly