Page 233 - Read Online
P. 233
Shibata Living donor liver transplantation anastomotic stenosis interventional radiology balloon dilatation
1.0 100
90
0.8 80
70
Patency rate 0.6 Patency rate (%) 60
50
0.4
40
30
0.2 20
10
0.0 0
0 50 100 150 200 0 50 100 150 200 250
Months after initial balloon dilatation Months after initial percutaneous intervention
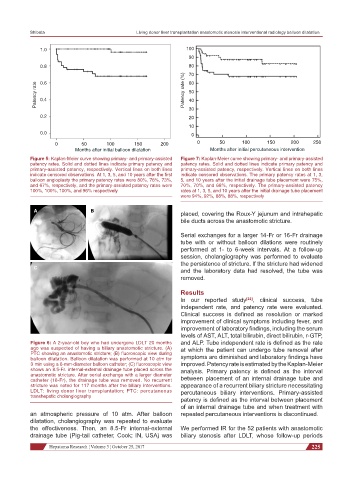
Figure 5: Kaplan-Meier curve showing primary- and primary-assisted Figure 7: Kaplan-Meier curve showing primary- and primary-assisted
patency rates. Solid and dotted lines indicate primary patency and patency rates. Solid and dotted lines indicate primary patency and
primary-assisted patency, respectively. Vertical lines on both lines primary-assisted patency, respectively. Vertical lines on both lines
indicate censored observations. At 1, 3, 5, and 10 years after the first indicate censored observations. The primary patency rates at 1, 3,
balloon angioplasty the primary patency rates were 80%, 76%, 73%, 5, and 10 years after the initial drainage tube placement were 75%,
and 67%, respectively, and the primary-assisted patency rates were 70%, 70%, and 68%, respectively. The primary-assisted patency
100%, 100%, 100%, and 96% respectively rates at 1, 3, 5, and 10 years after the initial drainage tube placement
were 94%, 92%, 88%, 88%, respectively
A B placed, covering the Roux-Y jejunum and intrahepatic
bile ducts across the anastomotic stricture.
Serial exchanges for a larger 14-Fr or 16-Fr drainage
tube with or without balloon dilations were routinely
performed at 1- to 6-week intervals. At a follow-up
session, cholangiography was performed to evaluate
the persistence of stricture. If the stricture had widened
C
and the laboratory data had resolved, the tube was
removed.
Results
In our reported study [22] , clinical success, tube
independent rate, and patency rate were evaluated.
Clinical success is defined as resolution or marked
improvement of clinical symptoms including fever, and
improvement of laboratory findings, including the serum
levels of AST, ALT, total bilirubin, direct bilirubin, r-GTP,
Figure 6: A 2-year-old boy who had undergone LDLT 20 months and ALP. Tube independent rate is defined as the rate
ago was suspected of having a biliary anastomotic stricture. (A) at which the patient can undergo tube removal after
PTC showing an anastomotic stricture; (B) fluoroscopic view during
balloon dilatation. Balloon dilatation was performed at 10 atm for symptoms are diminished and laboratory findings have
3 min using a 6-mm-diameter balloon catheter; (C) fluoroscopic view improved. Patency rate is estimated by the Kaplan-Meier
shows an 8.5-Fr. internal-external drainage tube placed across the analysis. Primary patency is defined as the interval
anastomotic stricture. After serial exchange with a larger diameter
catheter (16-Fr), the drainage tube was removed. No recurrent between placement of an internal drainage tube and
stricture was noted for 117 months after the biliary interventions. appearance of a recurrent biliary stricture necessitating
LDLT: living donor liver transplantation; PTC: percutaneous percutaneous biliary interventions. Primary-assisted
transhepatic cholangiography
patency is defined as the interval between placement
of an internal drainage tube and when treatment with
an atmospheric pressure of 10 atm. After balloon repeated percutaneous interventions is discontinued.
dilatation, cholangiography was repeated to evaluate
the effectiveness. Then, an 8.5-Fr internal-external We performed IR for the 52 patients with anastomotic
drainage tube (Pig-tail catheter, Cook; IN, USA) was biliary stenosis after LDLT, whose follow-up periods
Hepatoma Research ¦ Volume 3 ¦ October 25, 2017 225