Page 232 - Read Online
P. 232
Shibata Living donor liver transplantation anastomotic stenosis interventional radiology balloon dilatation
IR FOR ANASTOMOTIC BILIARY STENOSIS
A B
Anastomotic biliary stricture is the most common biliary
complication. Some studies have suggested that biliary
stricture occurs more frequently in post-LDLT patients
than in deceased liver transplantation because of the
small diameter of the anastomotic portion of the bile
duct, anatomical diversity of the bile ducts, or the
complicated nature of the surgical procedure [9,10,18] .
There are two strategies for treating anastomotic
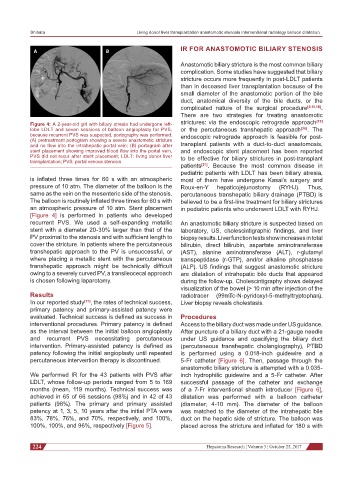
Figure 4: A 2-year-old girl with biliary atresia had undergone left- strictures: via the endoscopic retrograde approach [19]
lobe LDLT and seven sessions of balloon angioplasty for PVS, or the percutaneous transhepatic approach [20] . The
because recurrent PVS was suspected, portography was performed. endoscopic retrograde approach is feasible for post-
(A) pretreatment portogram showing a severe anastomotic stricture
and no flow into the intrahepatic portal vein; (B) portogram after transplant patients with a duct-to-duct anastomosis,
stent placement showing improved blood flow into the portal vein, and endoscopic stent placement has been reported
PVS did not recur after stent placement; LDLT: living donor liver to be effective for biliary strictures in post-transplant
transplantation; PVS: portal venous stenosis
patients [21] . Because the most common disease in
pediatric patients with LDLT has been biliary atresia,
is inflated three times for 60 s with an atmospheric most of them have undergone Kasai’s surgery and
pressure of 10 atm. The diameter of the balloon is the Roux-en-Y hepaticojejunostomy (RYHJ). Thus,
same as the vein on the mesenteric side of the stenosis. percutaneous transhepatic biliary drainage (PTBD) is
The balloon is routinely inflated three times for 60 s with believed to be a first-line treatment for biliary strictures
an atmospheric pressure of 10 atm. Stent placement in pediatric patients who underwent LDLT with RYHJ.
[Figure 4] is performed in patients who developed
recurrent PVS. We used a self-expanding metallic An anastomotic biliary stricture is suspected based on
stent with a diameter 20-30% larger than that of the laboratory, US, cholescintigraphic findings, and liver
PV proximal to the stenosis and with sufficient length to biopsy results. Liver function tests show increases in total
cover the stricture. In patients where the percutaneous bilirubin, direct bilirubin, aspartate aminotransferase
transhepatic approach to the PV is unsuccessful, or (AST), alanine aminotransferase (ALT), r-glutamyl
where placing a metallic stent with the percutaneous transpeptidase (r-GTP), and/or alkaline phosphatase
transhepatic approach might be technically difficult (ALP). US findings that suggest anastomotic stricture
owing to a severely curved PV, a transileocecal approach are dilatation of intrahepatic bile ducts that appeared
is chosen following laparotomy. during the follow-up. Cholescintigraphy shows delayed
visualization of the bowel (> 10 min after injection of the
Results radiotracer (99mTc-N-pyridoxyl-5-methyltryptophan).
In our reported study [17] , the rates of technical success, Liver biopsy reveals cholestasis.
primary patency and primary-assisted patency were
evaluated. Technical success is defined as success in Procedures
interventional procedures. Primary patency is defined Access to the biliary duct was made under US guidance.
as the interval between the initial balloon angioplasty After puncture of a biliary duct with a 21-gauge needle
and recurrent PVS necessitating percutaneous under US guidance and opacifying the biliary duct
intervention. Primary-assisted patency is defined as (percutaneous transhepatic cholangiography), PTBD
patency following the initial angioplasty until repeated is performed using a 0.018-inch guidewire and a
percutaneous intervention therapy is discontinued. 5-Fr catheter [Figure 6]. Then, passage through the
anastomotic biliary stricture is attempted with a 0.035-
We performed IR for the 43 patients with PVS after inch hydrophilic guidewire and a 5-Fr catheter. After
LDLT, whose follow-up periods ranged from 5 to 169 successful passage of the catheter and exchange
months (mean, 119 months). Technical success was of a 7-Fr interventional sheath introducer [Figure 6],
achieved in 65 of 66 sessions (98%) and in 42 of 43 dilatation was performed with a balloon catheter
patients (98%). The primary and primary assisted (diameter; 4-10 mm). The diameter of the balloon
patency at 1, 3, 5, 10 years after the initial PTA were was matched to the diameter of the intrahepatic bile
83%, 78%, 76%, and 70%, respectively, and 100%, duct on the hepatic side of stricture. The balloon was
100%, 100%, and 96%, respectively [Figure 5]. placed across the stricture and inflated for 180 s with
224 Hepatoma Research ¦ Volume 3 ¦ October 25, 2017