Page 49 - Read Online
P. 49
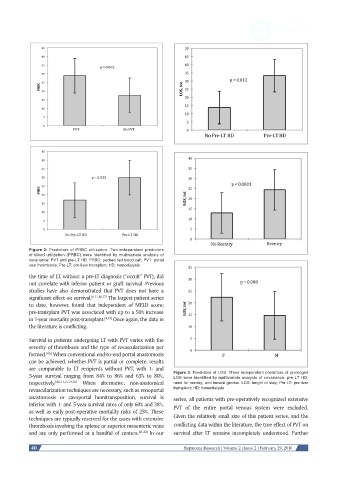
Figure 2: Predictors of PRBC utilization. Two independent predictors
of blood utilization (PRBC) were identified by multivariate analysis of
covariance: PVT and pre-LT HD. PRBC: packed red blood cell; PVT: portal
vein thrombosis; Pre-LT: pre-liver transplant; HD: hemodialysis
the time of LT, without a pre-LT diagnosis (“occult” PVT), did
not correlate with inferior patient or graft survival. Previous
studies have also demonstrated that PVT does not have a
significant effect on survival. [6,11,16,17] The largest patient series
to date, however, found that independent of MELD score;
pre-transplant PVT was associated with up to a 50% increase
in 1-year mortality post-transplant. [4,18] Once again, the data in
the literature is conflicting.
Survival in patients undergoing LT with PVT varies with the
severity of thrombosis and the type of revascularization per
formed. When conventional end-to-end portal anastomosis
[4,6]
can be achieved, whether PVT is partial or complete, results
are comparable to LT recipients without PVT, with 1- and
5-year survival ranging from 84% to 86% and 65% to 80%, Figure 3: Predictors of LOS. Three independent predictors of prolonged
LOS were identified by multivariate analysis of covariance: pre-LT HD,
respectively. [4,6,11,16,19,20] When alternative, non-anatomical need for reentry, and female gender. LOS: length of stay; Pre-LT: pre-liver
revascularization techniques are necessary, such as renoportal transplant; HD: hemodialysis
anastomosis or cavoportal hemitransposition, survival is series, all patients with pre-operatively recognized extensive
inferior with 1- and 5-year survival rates of only 60% and 38%, PVT of the entire portal venous system were excluded.
as well as early post-operative mortality risks of 25%. These
techniques are typically reserved for the cases with extensive Given the relatively small size of this patient series, and the
thrombosis involving the splenic or superior mesenteric veins conflicting data within the literature, the true effect of PVT on
and are only performed at a handful of centers. [21-23] In our survival after LT remains incompletely understood. Further
40 Hepatoma Research | Volume 2 | Issue 2 | February 29, 2016