Page 48 - Read Online
P. 48
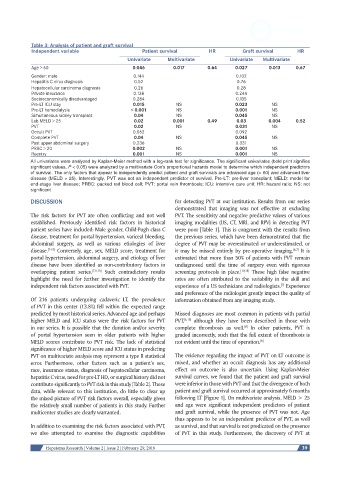
Table 3: Analysis of patient and graft survival
Independent variable Patient survival HR Graft survival HR
Univariate Multivariate Univariate Multivariate
Age > 60 0.046 0.017 0.64 0.027 0.013 0.67
Gender: male 0.144 0.102
Hepatitis C virus diagnosis 0.52 0.76
Hepatocellular carcinoma diagnosis 0.26 0.28
Private insurance 0.138 0.244
Socioeconomically disadvantaged 0.284 0.135
Pre-LT ICU stay 0.015 NS 0.023 NS
Pre-LT hemodialysis < 0.001 NS 0.001 NS
Simultaneous kidney transplant 0.04 NS 0.045 NS
Lab MELD > 25 0.02 0.001 0.49 0.03 0.004 0.52
PVT 0.02 NS 0.031 NS
Occult PVT 0.062 0.092
Complete PVT 0.04 NS 0.045 NS
Past upper abdominal surgery 0.236 0.331
PRBC > 20 0.002 NS 0.001 NS
Reentry 0.001 NS 0.001 NS
All univariates were analyzed by Kaplan-Meier method with a log-rank test for significance. The significant univariates (bold print signifies
significant values, P < 0.05) were analyzed by a multivariate Cox’s proportional hazards model to determine which independent predictors
of survival. The only factors that appear to independently predict patient and graft survivals are advanced age (> 60) and advanced liver
disease (MELD > 25). Interestingly, PVT was not an independent predictor of survival. Pre-LT: pre-liver transplant; MELD: model for
end-stage liver disease; PRBC: packed red blood cell; PVT: portal vein thrombosis; ICU: intensive care unit; HR: hazard ratio; NS: not
significant
DISCUSSION for detecting PVT at our institution. Results from our series
demonstrated that imaging was not effective at excluding
The risk factors for PVT are often conflicting and not well PVT. The sensitivity and negative predictive values of various
established. Previously identified risk factors in historical imaging modalities (US, CT, MRI, and RPV) in detecting PVT
patient series have included: Male gender, Child-Pugh class C were poor [Table 1]. This is congruent with the results from
disease, treatment for portal hypertension, variceal bleeding, the previous series, which have been demonstrated that the
abdominal surgery, as well as various etiologies of liver degree of PVT may be overestimated or underestimated, or
disease. [7-10] Conversely, age, sex, MELD score, treatment for it may be missed entirely by pre-operative imaging. It is
[6,7]
portal hypertension, abdominal surgery, and etiology of liver estimated that more than 50% of patients with PVT remain
disease have been identified as non-contributory factors in undiagnosed until the time of surgery even with rigorous
overlapping patient series. [7,9,10] Such contradictory results screening protocols in place. [10,11] These high false negative
highlight the need for further investigation to identify the rates are often attributed to the variability in the skill and
independent risk factors associated with PVT. experience of a US technicians and radiologists. Experience
[7]
and preference of the radiologist greatly impact the quality of
Of 216 patients undergoing cadaveric LT, the prevalence information obtained from any imaging study.
of PVT in this center (13.8%) fell within the expected range
predicted by most historical series. Advanced age and perhaps Missed diagnoses are most common in patients with partial
higher MELD and ICU status were the risk factors for PVT PVT, [6,15] although they have been described in those with
in our series. It is possible that the duration and/or severity complete thrombosis as well. In other patients, PVT is
[8]
of portal hypertension seen in older patients with higher graded incorrectly, such that the full extent of thrombosis is
MELD scores contribute to PVT risk. The lack of statistical not evident until the time of operation. [6]
significance of higher MELD score and ICU status in predicting
PVT on multivariate analysis may represent a type II statistical The evidence regarding the impact of PVT on LT outcome is
error. Furthermore, other factors such as a patient’s sex, mixed, and whether an occult diagnosis has any additional
race, insurance status, diagnosis of hepatocellular carcinoma, effect on outcome is also uncertain. Using Kaplan-Meier
hepatitis C virus, need for pre-LT HD, or surgical history did not survival curves, we found that the patient and graft survival
contribute significantly to PVT risk in this study [Table 2]. These were inferior in those with PVT and that the divergence of both
data, while relevant to this institution, do little to clear up patient and graft survival occurred at approximately 6 months
the mixed picture of PVT risk factors overall, especially given following LT [Figure 1]. On multivariate analysis, MELD > 25
the relatively small number of patients in this study. Further and age were significant independent predictors of patient
multicenter studies are clearly warranted. and graft survival, while the presence of PVT was not. Age
thus appears to be an independent predictor of PVT, as well
In addition to examining the risk factors associated with PVT, as survival, and that survival is not predicated on the presence
we also attempted to examine the diagnostic capabilities of PVT in this study. Furthermore, the discovery of PVT at
Hepatoma Research | Volume 2 | Issue 2 | February 29, 2016 39