Page 297 - Read Online
P. 297
Lei et al. HLH presenting as ACS
[2]
throughput sequencing. The mutations in adult HLH, A
[3]
when present, are less likely to be bi-allelic. From
the genetic point of view, adult or secondary HLH
[4]
cases are intrinsically different. Because HLH-2004
diagnostic guidelines were established for pediatric
cases, it has always been a question whether or not
HLH-2004 can be readily applied to adult patients.
It is important yet challenging to recognize HLH in
a timely manner because HLH can be quickly fatal
without prompt diagnosis and treatment, but the
presenting symptoms are often nonspecific. We
herein present a fulminant fatal case in an elderly B
female with an unusual presentation of abdominal
compartment syndrome (ACS), and review recent
advances in diagnosing adult HLH.
CASE REPORT
The patient was a previously healthy, 65-year-old
female who presented with fever and chills for 4 days,
and mild right upper quadrant abdominal pain for 1
day. Complete blood count (CBC) showed neutropenia
9
9
(1.4 × 10 /L) and thrombocytopenia (72 × 10 /L), which
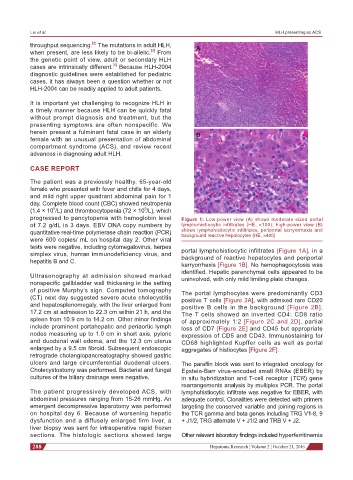
progressed to pancytopenia with hemoglobin level Figure 1: Low-power view (A) shows moderate-sized portal
of 7.2 g/dL in 3 days. EBV DNA copy numbers by lymphohistiocytic infiltrates (HE, ×100); high-power view (B)
quantitative real-time polymerase chain reaction (PCR) shows lymphohistiocytic infiltrates, periportal karryorrhexis and
background reactive hepatocytes (HE, ×400)
were 600 copies/ mL on hospital day 2. Other viral
tests were negative, including cytomegalovirus, herpes portal lymphohistiocytic infiltrates [Figure 1A], in a
simplex virus, human immunodeficiency virus, and background of reactive hepatocytes and periportal
hepatitis B and C.
karryorrhexis [Figure 1B]. No hemophagocytosis was
identified. Hepatic parenchymal cells appeared to be
Ultrasonography at admission showed marked uninvolved, with only mild limiting plate changes.
nonspecific gallbladder wall thickening in the setting
of positive Murphy’s sign. Computed tomography The portal lymphocytes were predominantly CD3
(CT) next day suggested severe acute cholecystitis positive T cells [Figure 2A], with admixed rare CD20
and hepatosplenomegaly, with the liver enlarged from positive B cells in the background [Figure 2B].
17.2 cm at admission to 22.3 cm within 21 h, and the The T cells showed an inverted CD4: CD8 ratio
spleen from 10.9 cm to 14.2 cm. Other minor findings of approximately 1:2 [Figure 2C and 2D], partial
include prominent portahepatic and periaortic lymph loss of CD7 [Figure 2E] and CD45 but appropriate
nodes measuring up to 1.0 cm in short axis, pyloric expression of CD5 and CD43. Immunostaining for
and duodenal wall edema, and the 12.3 cm uterus CD68 highlighted Kupffer cells as well as portal
enlarged by a 9.5 cm fibroid. Subsequent endoscopic aggregates of histiocytes [Figure 2F].
retrograde cholangiopancreatography showed gastric
ulcers and large circumferential duodenal ulcers. The paraffin block was sent to integrated oncology for
Cholecystostomy was performed. Bacterial and fungal Epstein-Barr virus-encoded small RNAs (EBER) by
cultures of the biliary drainage were negative. in situ hybridization and T-cell receptor (TCR) gene
rearrangements analysis by multiplex PCR. The portal
The patient progressively developed ACS, with lymphohistiocytic infiltrate was negative for EBER, with
abdominal pressures ranging from 15-26 mmHg. An adequate control. Clonalities were detected with primers
emergent decompressive laparotomy was performed targeting the conserved variable and joining regions in
on hospital day 6. Because of worsening hepatic the TCR gamma and beta genes including TRG V1-8, 9
dysfunction and a diffusely enlarged firm liver, a + J1/2, TRG alternate V + J1/2 and TRB V + J2.
liver biopsy was sent for intraoperative rapid frozen
sections. The histologic sections showed large Other relevant laboratory findings included hyperferritinemia
288 Hepatoma Research ¦ Volume 2 ¦ October 21, 2016