Page 63 - Read Online
P. 63
Morgan et al. Vessel Plus 2020;4:6 I http://dx.doi.org/10.20517/2574-1209.2019.32 Page 5 of 14
A B
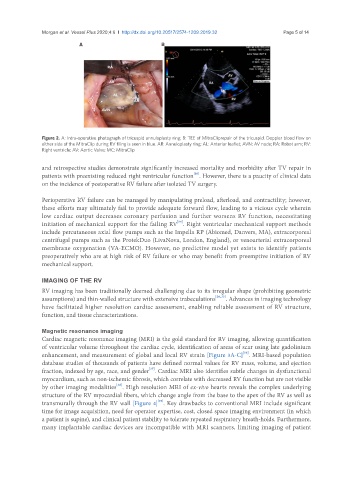
Figure 2. A: Intra-operative photograph of tricuspid annuloplasty ring; B: TEE of MitraCliprepair of the tricuspid. Doppler blood flow on
either side of the MitraClip during RV flling is seen in blue. AR: Annuloplasty ring; AL: Anterior leaflet; AVN: AV node; RA: Robot arm; RV:
Right ventricle; AV: Aortic Valve; MC: MitraClip
and retrospective studies demonstrate significantly increased mortality and morbidity after TV repair in
[10]
patients with preexisting reduced right ventricular function . However, there is a paucity of clinical data
on the incidence of postoperative RV failure after isolated TV surgery.
Perioperative RV failure can be managed by manipulating preload, afterload, and contractility; however,
these efforts may ultimately fail to provide adequate forward flow, leading to a vicious cycle wherein
low cardiac output decreases coronary perfusion and further worsens RV function, necessitating
[34]
initiation of mechanical support for the failing RV . Right ventricular mechanical support methods
include percutaneous axial flow pumps such as the Impella RP (Abiomed, Danvers, MA), extracorporeal
centrifugal pumps such as the ProtekDuo (LivaNova, London, England), or venoarterial extracorporeal
membrane oxygenation (VA-ECMO). However, no predictive model yet exists to identify patients
preoperatively who are at high risk of RV failure or who may benefit from preemptive initiation of RV
mechanical support.
IMAGING OF THE RV
RV imaging has been traditionally deemed challenging due to its irregular shape (prohibiting geometric
assumptions) and thin-walled structure with extensive trabeculations [26,35] . Advances in imaging technology
have facilitated higher resolution cardiac assessment, enabling reliable assessment of RV structure,
function, and tissue characterizations.
Magnetic resonance imaging
Cardiac magnetic resonance imaging (MRI) is the gold standard for RV imaging, allowing quantification
of ventricular volume throughout the cardiac cycle, identification of areas of scar using late gadolinium
[36]
enhancement, and measurement of global and local RV strain [Figure 3A-C] . MRI-based population
database studies of thousands of patients have defined normal values for RV mass, volume, and ejection
[37]
fraction, indexed by age, race, and gender . Cardiac MRI also identifies subtle changes in dysfunctional
myocardium, such as non-ischemic fibrosis, which correlate with decreased RV function but are not visible
[38]
by other imaging modalities . High resolution MRI of ex-vivo hearts reveals the complex underlying
structure of the RV myocardial fibers, which change angle from the base to the apex of the RV as well as
[39]
transmurally through the RV wall [Figure 4] . Key drawbacks to conventional MRI include significant
time for image acquisition, need for operator expertise, cost, closed space imaging environment (in which
a patient is supine), and clinical patient stability to tolerate repeated respiratory breath-holds. Furthermore,
many implantable cardiac devices are incompatible with MRI scanners, limiting imaging of patient