Page 381 - Read Online
P. 381
Fang et al. Negative pressure wound therapy for diabetic foot limb salvage
A B
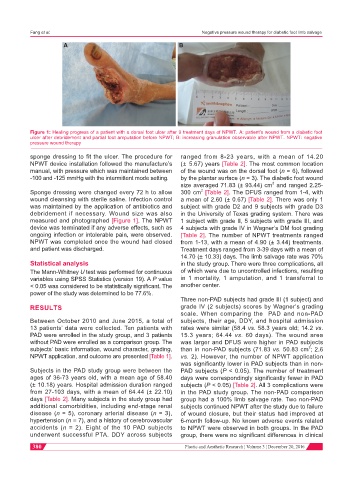
Figure 1: Healing progress of a patient with a dorsal foot ulcer after 9 treatment days of NPWT. A: patient’s wound from a diabetic foot
ulcer after debridement and partial foot amputation before NPWT; B: increasing granulation observable after NPWT. NPWT: negative
pressure wound therapy
sponge dressing to fit the ulcer. The procedure for ranged from 8-23 years, with a mean of 14.20
NPWT device installation followed the manufacture’s (± 5.67) years [Table 2]. The most common location
manual, with pressure which was maintained between of the wound was on the dorsal foot (n = 6), followed
-100 and -125 mmHg with the intermittent mode setting. by the plantar surface (n = 3). The diabetic foot wound
2
size averaged 71.83 (± 93.44) cm and ranged 2.25-
2
Sponge dressing were changed every 72 h to allow 300 cm [Table 2]. The DFUS ranged from 1-4, with
wound cleansing with sterile saline. Infection control a mean of 2.60 (± 0.67) [Table 2]. There was only 1
was maintained by the application of antibiotics and subject with grade D2 and 9 subjects with grade D3
debridement if necessary. Wound size was also in the University of Texas grading system. There was
measured and photographed [Figure 1]. The NPWT 1 subject with grade II, 5 subjects with grade III, and
device was terminated if any adverse effects, such as 4 subjects with grade IV in Wagner’s DM foot grading
ongoing infection or intolerable pain, were observed. [Table 2]. The number of NPWT treatments ranged
NPWT was completed once the wound had closed from 1-13, with a mean of 4.90 (± 3.44) treatments.
and patient was discharged. Treatment days ranged from 3-39 days with a mean of
14.70 (± 10.33) days. The limb salvage rate was 70%
Statistical analysis in the study group. There were three complications, all
The Mann-Whitney U test was performed for continuous of which were due to uncontrolled infections, resulting
variables using SPSS Statistics (version 19). A P value in 1 mortality, 1 amputation, and 1 transferral to
< 0.05 was considered to be statistically significant. The another center.
power of the study was determined to be 77.6%.
Three non-PAD subjects had grade III (1 subject) and
RESULTS grade IV (2 subjects) scores by Wagner’s grading
scale. When comparing the PAD and non-PAD
Between October 2010 and June 2015, a total of subjects, their age, DDY, and hospital admission
13 patients’ data were collected. Ten patients with rates were similar (58.4 vs. 58.3 years old; 14.2 vs.
PAD were enrolled in the study group, and 3 patients 15.3 years; 64.44 vs. 60 days). The wound area
without PAD were enrolled as a comparison group. The was larger and DFUS were higher in PAD subjects
2
subjects’ basic information, wound character, grading, than in non-PAD subjects (71.83 vs. 50.83 cm ; 2.6
NPWT application, and outcome are presented [Table 1]. vs. 2). However, the number of NPWT application
was significantly lower in PAD subjects than in non-
Subjects in the PAD study group were between the PAD subjects (P < 0.05). The number of treatment
ages of 36-73 years old, with a mean age of 58.40 days were correspondingly significantly fewer in PAD
(± 10.18) years. Hospital admission duration ranged subjects (P < 0.05) [Table 2]. All 3 complications were
from 27-103 days, with a mean of 64.44 (± 22.10) in the PAD study group. The non-PAD comparison
days [Table 2]. Many subjects in the study group had group had a 100% limb salvage rate. Two non-PAD
additional comorbidities, including end-stage renal subjects continued NPWT after the study due to failure
disease (n = 5), coronary arterial disease (n = 3), of wound closure, but their status had improved at
hypertension (n = 7), and a history of cerebrovascular 6-month follow-up. No known adverse events related
accidents (n = 2). Eight of the 10 PAD subjects to NPWT were observed in both groups. In the PAD
underwent successful PTA. DDY across subjects group, there were no significant differences in clinical
380 Plastic and Aesthetic Research ¦ Volume 3 ¦ December 20, 2016