Page 212 - Read Online
P. 212
Infante et al. PML after rituximab
INTRODUCTION He was treated with chlorambucil in 2012, followed
by 6 cycles of fludarabine, cyclophosphamide and
Progressive multifocal encephalopathy (PML) is a lenalidomide in 2013, with complete response; he was
demyelinating infectious disease of the central nervous then treated with rituximab and steroids for hemolytic
system caused by reactivation of John Cunningham anemia (for 4 weeks in 2014) with complete regression.
polyomavirus (JCV) and often leads to death resulting
from progressive oligodendrocytes infection and In March 2016, he was admitted to the emergency
lysis . Prior to human immunodeficiency virus era, department for acute dizziness and ataxia followed,
[1]
this infection was seen in severely immunosuppressed after one day, by dysarthria and left limbs ataxia. A
patients, including individuals with hematological cerebral unenhanced computed tomography (CT)
malignancies, organ transplantation or chronic
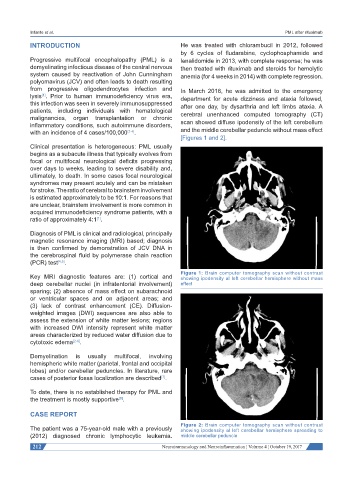
inflammatory conditions, such autoimmune disorders, scan showed diffuse ipodensity of the left cerebellum
with an incidence of 4 cases/100,000 [2-4] . and the middle cerebellar peduncle without mass effect
[Figures 1 and 2].
Clinical presentation is heterogeneous: PML usually
begins as a subacute illness that typically evolves from
focal or multifocal neurological deficits progressing
over days to weeks, leading to severe disability and,
ultimately, to death. In some cases focal neurological
syndromes may present acutely and can be mistaken
for stroke. The ratio of cerebral to brainstem involvement
is estimated approximately to be 10:1. For reasons that
are unclear, brainstem involvement is more common in
acquired immunodeficiency syndrome patients, with a
ratio of approximately 4:1 .
[1]
Diagnosis of PML is clinical and radiological, principally
magnetic resonance imaging (MRI) based; diagnosis
is then confirmed by demonstration of JCV DNA in
the cerebrospinal fluid by polymerase chain reaction
(PCR) test [4,5] .
Figure 1: Brain computer tomography scan without contrast
Key MRI diagnostic features are: (1) cortical and showing ipodensity al left cerebellar hemisphere without mass
deep cerebellar nuclei (in infratentorial involvement) effect
sparing; (2) absence of mass effect on subarachnoid
or ventricular spaces and on adjacent areas; and
(3) lack of contrast enhancement (CE). Diffusion-
weighted images (DWI) sequences are also able to
assess the extension of white matter lesions; regions
with increased DWI intensity represent white matter
areas characterized by reduced water diffusion due to
cytotoxic edema [2-6] .
Demyelination is usually multifocal, involving
hemispheric white matter (parietal, frontal and occipital
lobes) and/or cerebellar peduncles. In literature, rare
cases of posterior fossa localization are described .
[7]
To date, there is no established therapy for PML and
the treatment is mostly supportive .
[8]
CASE REPORT
The patient was a 75-year-old male with a previously Figure 2: Brain computer tomography scan without contrast
showing ipodensity al left cerebellar hemisphere spreading to
(2012) diagnosed chronic lymphocytic leukemia. middle cerebellar peduncle
212 Neuroimmunology and Neuroinflammation ¦ Volume 4 ¦ October 19, 2017