Page 217 - Read Online
P. 217
Meenakshi-Sundaram et al. Stroke thrombolysis in a patient on prasugrel
INTRODUCTION the onset of stroke, revealed a moderate sized infarct
involving the left middle cerebral artery territory
Intravenous thrombolysis is the standard of care in [Figure 1A and B]. MR angiogram revealed diffuse
acute ischemic stroke, and is associated with significant pruning of M1 and significant reduction of signals in
improvement in outcome measures . Intracerebral M2 and M3 segments [Figure 1C]. Echocardiogram
[1]
hemorrhage is an absolute contraindication for revealed no intracardiac clot.
thrombolysis. While due diligence must be exercised,
strict interpretations of relative contraindications The risks and benefits of intravenous thrombolysis
might prove a barrier to potentially life changing were discussed with the family. After obtaining
thrombolysis in stroke [2,3] . Hence decisions regarding informed consent alteplase was administered. Stroke-
thrombolysis are made on a case-by-case basis . onset to needle-time was 55 min. Following the bolus
[4]
We report a patient who, whilst on prasugrel and of 5.5 mg, a mild improvement in motor power was
aspirin for post-myocardial infarction (MI), made a noted when he could minimally move the right lower
dramatic recovery from acute ischemic stroke after limb. There was a gradual improvement of limb power
thrombolysis. during the infusion of alteplase. He developed an
oral bleed after 29 mg of the drug had been infused.
CASE REPORT Further infusion was discontinued. Limb power
improved to grade 3/5 over the upper and lower limbs,
A 55-year-old gentleman was referred to our hospital and verbal comprehension was normal. However, he
two days following the development of inferior wall continued to have Broca’s aphasia. CT scan of the
myocardial infarction (IWMI) diagnosed as ST- brain, done immediately, did not reveal intracerebral
elevation myocardial infarction (STEMI) that had hemorrhage. No further administration of alteplase
been treated with antiplatelets and statin. The last was done. Fifteen minutes post thrombolysis Broca’s
ECG at the time of discharge after the IWMI revealed aphasia also significantly improved and he could
evolved infarction. Three days after the onset of IWMI speak several words fluently. NIHSS was 5. Twelve
he underwent percutaneous angioplasty of the right hours post thrombolysis, NIHSS was zero. Repeat CT
coronary artery. Three days following this procedure, scan did not reveal any hemorrhagic complications.
he was discharged on the following medications: Aspirin, 150 mg/day, was started after 24 h and
aspirin 150 mg/day, prasugrel 10 mg/day, and clopidogrel, 75 mg/day, after 48 h. He maintained
atorvastatin 40 mg/day. While being discharged he improvement and was discharged 4 days after the
developed weakness of right sided limbs, inability to onset of stroke.
comprehend or talk, and became drowsy. There was
no history of headache, vomiting, or convulsions. At DISCUSSION
the emergency room, his vital parameters were: BP
110/60 mmHg, pulse 64/min. He had global aphasia, Alteplase is the only approved intravenous
right gaze palsy, right hemiplegia, hemianopia, thrombolytic therapy for stroke and is recommended
hemihypoaesthesia, and sensory inattention. National in the first 4.5 h following the onset of acute ischemic
Institute of Health Stroke Scale (NIHSS) was 28. stroke . Contraindications to its use were derived
[1]
Blood sugar was 160 mg%. CT scan of the brain was from the exclusion criteria utilized in major stroke
unremarkable. MRI of the brain, done 30 min after trials, and violation of protocols have been shown
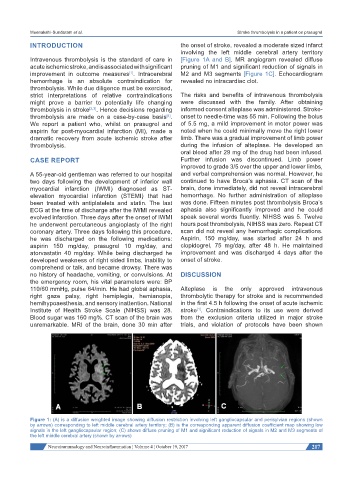
Figure 1: (A) is a diffusion weighted image showing diffusion restriction involving left gangliocapsular and perisylvian regions (shown
by arrows) corresponding to left middle cerebral artery territory; (B) is the corresponding apparent diffusion coefficient map showing low
signals in the left gangliocapsular region; (C) shows diffuse pruning of M1 and significant reduction of signals in M2 and M3 segments of
the left middle cerebral artery (shown by arrows)
Neuroimmunology and Neuroinflammation ¦ Volume 4 ¦ October 19, 2017 217