Page 213 - Read Online
P. 213
Infante et al. PML after rituximab
Neurological examination showed that the patient bands on cerebrospinal fluid (CSF) and serum, PCR for
had dysarthria and left limbs dysmetria, left-beating neurotropic viruses (HSV, VZV, CMV, EBV, Adenovirus
nystagmus and balance difficulties. Acute ischemic and Enterovirus) and cultural CSF examination were
stroke was suspected and antiplatelets therapy negative. A broad-spectrum antiviral and antibacterial
with aspirin was started, with transitory symptoms therapy was started without improvement. Blood test
improvement. exams were normal.
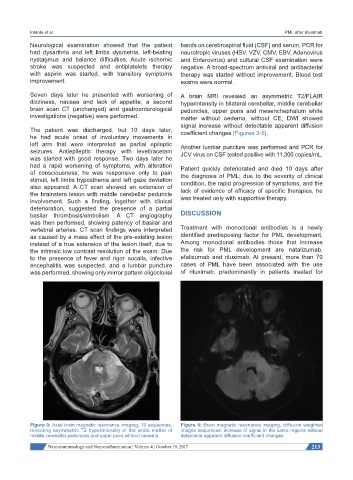
Seven days later he presented with worsening of A brain MRI revealed an asymmetric T2/FLAIR
dizziness, nausea and lack of appetite; a second hyperintensity in bilateral cerebellar, middle cerebellar
brain scan CT (unchanged) and gastroenterological peduncles, upper pons and mesenchephalum white
investigations (negative) were performed. matter without oedema, without CE; DWI showed
signal increase without detectable apparent diffusion
The patient was discharged, but 10 days later, coefficient changes [Figures 3-5].
he had acute onset of involuntary movements in
left arm that were interpreted as partial epileptic Another lumbar puncture was performed and PCR for
seizures. Antiepileptic therapy with levetiracetam JCV virus on CSF tested positive with 11,300 copies/mL.
was started with good response. Two days later he
had a rapid worsening of symptoms, with alteration Patient quickly deteriorated and died 10 days after
of consciousness; he was responsive only to pain the diagnosis of PML; due to the severity of clinical
stimuli, left limbs hyposthenia and left gaze deviation condition, the rapid progression of symptoms, and the
also appeared. A CT scan showed an extension of lack of evidence of efficacy of specific therapies, he
the brainstem lesion with middle cerebellar peduncle
involvement. Such a finding, together with clinical was treated only with supportive therapy.
deterioration, suggested the presence of a partial
basilar thrombosis/embolism. A CT angiography DISCUSSION
was then performed, showing patency of basilar and
vertebral arteries. CT scan findings were interpreted Treatment with monoclonal antibodies is a newly
as caused by a mass effect of the pre-existing lesion identified predisposing factor for PML development.
instead of a true extension of the lesion itself, due to Among monoclonal antibodies those that increase
the intrinsic low contrast resolution of the exam. Due the risk for PML development are natalizumab,
to the presence of fever and rigor nucalis, infective efalizumab and rituximab. At present, more than 70
encephalitis was suspected, and a lumbar puncture cases of PML have been associated with the use
was performed, showing only mirror pattern oligoclonal of rituximab, predominantly in patients treated for
Figure 3: Axial brain magnetic resonance imaging, T2 sequences, Figure 4: Brain magnetic resonance imaging, diffusion weighted
revealing asymmetric T2 hyperintensity of the white matter of images sequences: increase of signal in the same regions without
middle cerebellar peduncles and upper pons without oedema detectable apparent diffusion coefficient changes
Neuroimmunology and Neuroinflammation ¦ Volume 4 ¦ October 19, 2017 213