Page 267 - Read Online
P. 267
Liu et al. Anti-NMDAR encephlitis and ADEM-like findings
of autoimmune encephalitis was considered, and mental disorders, and autonomic instability; because
she was treated with high doses of intravenous such unusual symptoms may overlap anti-NMDAR
methylprednisolone (1 g/day for 3 days, 0.5 g/day for 2 encephalitis. There are several articles about this.
[5]
days, 0.25 g/day for 1 day) with two courses of treatment. Here, we report a middle-aged woman with NMDAR-
Abs and clinical and radiologic evidence of ADEM, as
The following tests were normal or negative: routine blood well as follow-up after treatment.
test, autoantibody screen, anti-neutrophil cytoplasmic
antibody, anti-nuclear antibodies, antibodies related Most patients with anti-NMDAR encephalitis will
to paraneoplastic neurologic system diseases, acute have complete or near-complete recovery. However,
flaccid paralysis, thyroid biochemistry and antibodies,
HIV, CA-125, chest X-ray, electrocardiograms,
abdomen and pelvic ultrasound, HBSAg (+), and PET-
CT showed tumor-negative. Serum and cerebrospinal
fluid (CSF) tested positive for anti-NMDAR (titers
1:10) (semiquantitative indirect fluorescent antibody,
EUROIMMUN Laboratories). On admission, lumbar
puncture (LP) initially showed CSF with a mildly raised
protein of 0.51 g/L, with 60 × 10 /L white blood cells,
6
2.16 mmol/L glucose. PCR for HSV, EBV, CMV in CSF,
and bacterial cultures of the CSF were negative. On
repeat testing 2 weeks later, LP showed the protein
had normalized, a white cell count of 18 × 10 /L, and
6
3.72 mmol/L glucose. Serum anti-neuromyelitis optica
(NMO)/aquaporin-4 (AQP4) antibody was negative.
Serum and CSF oligoclonal bands were positive.
Magnetic resonance imaging (MRI) brain scans
showed multiple areas of T2 hyperintensity within 1
month after onset and gradually evolving higher signals
in the cerebral hemispheres, medulla, cerebellum, and
C1-T6 spinal cord. MR scans showed disseminated
demyelination lesions on T2 imaging within 1.5 months
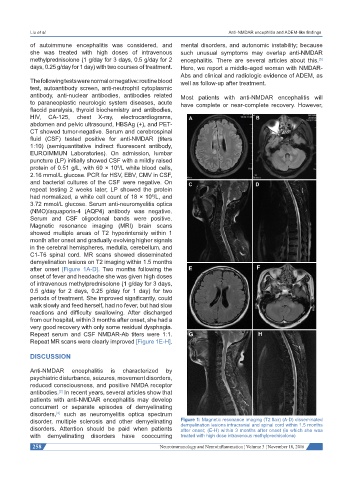
after onset [Figure 1A-D]. Two months following the
onset of fever and headache she was given high doses
of intravenous methylprednisolone (1 g/day for 3 days,
0.5 g/day for 2 days, 0.25 g/day for 1 day) for two
periods of treatment. She improved significantly, could
walk slowly and feed herself, had no fever, but had slow
reactions and difficulty swallowing. After discharged
from our hospital, within 3 months after onset, she had a
very good recovery with only some residual dysphagia.
Repeat serum and CSF NMDAR-Ab titers were 1:1.
Repeat MR scans were clearly improved [Figure 1E-H].
DISCUSSION
Anti-NMDAR encephalitis is characterized by
psychiatric disturbance, seizures, movement disorders,
reduced consciousness, and positive NMDA receptor
antibodies. In recent years, several articles show that
[2]
patients with anti-NMDAR encephalitis may develop
concurrent or separate episodes of demyelinating
disorders, such as neuromyelitis optica spectrum
[4]
disorder, multiple sclerosis and other demyelinating Figure 1: Magnetic resonance imaging (T2 flair) (A-D) disseminated
demyelination lesions intracranial and spinal cord within 1.5 months
disorders. Attention should be paid when patients after onset; (E-H) within 3 months after onset (in which she was
with demyelinating disorders have cooccurring treated with high dose intravenous methylprednisolone)
258 Neuroimmunology and Neuroinflammation ¦ Volume 3 ¦ November 18, 2016