Page 255 - Read Online
P. 255
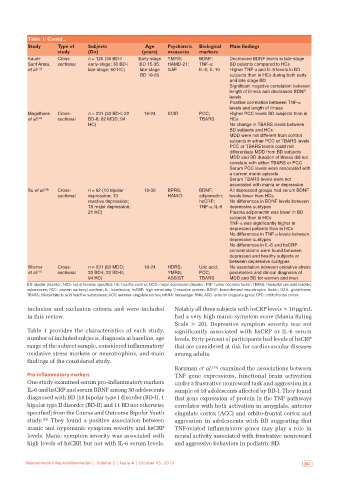
Table 1: Contd...
Study Type of Subjects Age Psychiatric Biological Main findings
study (Dx) (years) measures markers
Kauer‑ Cross‑ n = 120 (30 BD‑I Early‑stage YMRS; BDNF; Decreased BDNF levels in late‑stage
Sant’Anna, sectional early‑stage; 30 BD‑I BD 15‑35; HAMD‑21; TNF‑α; BD patients compared to HCs
et al. [10] late‑stage; 60 HC) late‑stage GAF IL‑6; IL‑10 Higher TNF‑α and IL‑6 levels in BD
BD 18‑65 subjects than in HCs during both early
and late stage BD
Significant negative correlation between
length of illness and decreased BDNF
levels
Positive correlation between TNF‑α
levels and length of illness
Magalhaes Cross‑ n = 231 (33 BD‑I; 22 18‑24 SCID PCC; Higher PCC levels BD subjects than in
et al. [40] sectional BD‑II; 82 MDD; 94 TBARS HCs
HC) No change in TBARS levels between
BD subjects and HCs
MDD were not different from control
subjects in either PCC or TBARS levels
PCC or TBARS levels could not
differentiate MDD from BD subjects
MDD and BD duration of illness did not
correlate with either TBARS or PCC
Serum PCC levels were associated with
a current manic episode
Serum TBARS levels were not
associated with mania or depression
Su et al. [36] Cross‑ n = 62 (10 bipolar 18‑30 BPRS; BDNF; All depressed groups had serum BDNF
sectional depression; 13 HAM‑D adiponectin; levels lower than HCs
reactive depression; hsCRP; No differences in BDNF levels between
18 major depression; TNF‑α; IL‑6 depressive subtypes
21 HC) Plasma adiponectin was lower in BD
subjects than in HCs
TNF‑α was significantly higher in
depressed patients than in HCs
No differences in TNF‑α levels between
depressive subtypes
No differences in IL‑6 and hsCRP
concentrations were found between
depressed and healthy subjects or
between depressive subtypes
Wiener Cross‑ n = 231 (82 MDD; 18‑24 HDRS; Uric acid; No association between oxidative stress
et al. [41] sectional 33 BD‑I; 22 BD‑II; YMRS; PCC; parameters and clinical diagnosis of
94 HC) ASSIST TBARS MDD and BD for women and men
BD: bipolar disorder; NOS: not otherwise specified; HC: healthy control; MDD: major depressive disorder; TNF: tumor necrosis factor; TBARS: thiobarbituric acid reactive
substances; PCC: protein carbonyl content; IL: interleukin; hsCRP: high‑sensitivity C‑reactive protein; BDNF: brain‑derived neurotrophic factor; GSH: glutathione;
TBARS: thiobarbituric acid reactive substances; ACC: anterior cingulate cortex; mRNA: messenger RNA; ACG: anterior cingulate gyrus; OFC: orbitofrontal cortex
inclusion and exclusion criteria and were included Notably all three subjects with hsCRP levels > 10 μg/mL
in this review. had a very high manic symptom score (Mania Rating
Scale > 20). Depressive symptom severity was not
Table 1 provides the characteristics of each study, significantly associated with hsCRP or IL‑6 serum
number of included subjects, diagnosis at baseline, age levels. Forty percent of participants had levels of hsCRP
range of the subject sample, considered inflammatory/ that are considered at risk for cardiovascular diseases
oxidative stress markers or neurotrophins, and main among adults.
findings of the considered study.
Barzman et al. [35] examined the associations between
Pro‑inflammatory markers TNF gene expressions, functional brain activation
One study examined serum pro‑inflammatory markers under a frustrative nonreward task and aggression in a
IL‑6 and hsCRP and serum BDNF among 30 adolescents sample of 10 adolescents affected by BD‑I. They found
diagnosed with BD [18 bipolar type I disorder (BD‑I), 1 that gene expression of protein in the TNF pathways
bipolar type II disorder (BD‑II) and 11 BD not otherwise correlates with both activation in amygdala, anterior
specified] from the Course and Outcome Bipolar Youth cingulate cortex (ACC) and orbito‑frontal cortex and
study. [29] They found a positive association between aggression in adolescents with BD suggesting that
manic and hypomanic symptom severity and hsCRP TNF‑related inflammatory genes may play a role in
levels. Manic symptom severity was associated with neural activity associated with frustrative nonreward
high levels of hsCRP, but not with IL‑6 serum levels. and aggressive behaviors in pediatric BD.
Neuroimmunol Neuroinflammation | Volume 2 | Issue 4 | October 15, 2015 247