Page 601 - Read Online
P. 601
Page 10 of 15 Saxena et al. Mini-invasive Surg 2020;4:62 I http://dx.doi.org/10.20517/2574-1225.2020.68
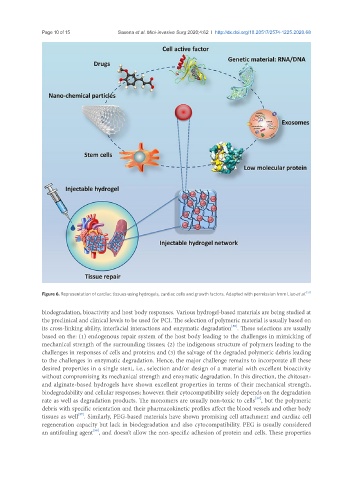
Figure 6. Representation of cardiac tissues using hydrogels, cardiac cells and growth factors. Adapted with permission from Liao et al. [51]
biodegradation, bioactivity and host body responses. Various hydrogel-based materials are being studied at
the preclinical and clinical levels to be used for PCI. The selection of polymeric material is usually based on
[56]
its cross-linking ability, interfacial interactions and enzymatic degradation . These selections are usually
based on the: (1) endogenous repair system of the host body leading to the challenges in mimicking of
mechanical strength of the surrounding tissues; (2) the indigenous structure of polymers leading to the
challenges in responses of cells and proteins; and (3) the salvage of the degraded polymeric debris leading
to the challenges in enzymatic degradation. Hence, the major challenge remains to incorporate all these
desired properties in a single stent, i.e., selection and/or design of a material with excellent bioactivity
without compromising its mechanical strength and enzymatic degradation. In this direction, the chitosan-
and alginate-based hydrogels have shown excellent properties in terms of their mechanical strength,
biodegradability and cellular responses; however, their cytocompatibility solely depends on the degradation
[32]
rate as well as degradation products. The monomers are usually non-toxic to cells , but the polymeric
debris with specific orientation and their pharmacokinetic profiles affect the blood vessels and other body
[57]
tissues as well . Similarly, PEG-based materials have shown promising cell attachment and cardiac cell
regeneration capacity but lack in biodegradation and also cytocompatibility. PEG is usually considered
an antifouling agent , and doesn’t allow the non-specific adhesion of protein and cells. These properties
[58]