Page 192 - Read Online
P. 192
Page 4 of 10 Zhao et al. Mini-invasive Surg 2018;2:26 I http://dx.doi.org/10.20517/2574-1225.2018.27
A B
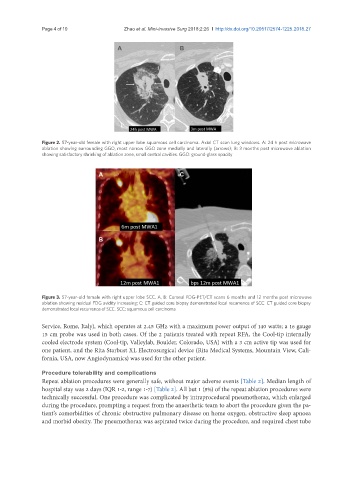
Figure 2. 57-year-old female with right upper lobe squamous cell carcinoma. Axial CT scan lung windows. A: 24 h post microwave
ablation showing surrounding GGO, most narrow GGO zone medially and laterally (arrows); B: 3 months post microwave ablation
showing satisfactory shrinking of ablation zone, small central cavities. GGO: ground-glass opacity
A C
B
Figure 3. 57-year-old female with right upper lobe SCC. A, B: Coronal FDG-PET/CT scans 6 months and 12 months post microwave
ablation showing residual FDG avidity increasing; C: CT guided core biopsy demonstrated local recurrence of SCC. CT guided core biopsy
demonstrated local recurrence of SCC. SCC: squamous cell carcinoma
Service, Rome, Italy), which operates at 2.45 GHz with a maximum power output of 140 watts; a 16 gauge
15 cm probe was used in both cases. Of the 2 patients treated with repeat RFA, the Cool-tip internally
cooled electrode system (Cool-tip, Valleylab, Boulder, Colorado, USA) with a 3 cm active tip was used for
one patient, and the Rita Starbust XL Electrosurgical device (Rita Medical Systems, Mountain View, Cali-
fornia, USA, now Angiodynamics) was used for the other patient.
Procedure tolerability and complications
Repeat ablation procedures were generally safe, without major adverse events [Table 2]. Median length of
hospital stay was 2 days (IQR 1-2, range 1-7) [Table 2]. All but 1 (8%) of the repeat ablation procedures were
technically successful. One procedure was complicated by intraprocedural pneumothorax, which enlarged
during the procedure, prompting a request from the anaesthetic team to abort the procedure given the pa-
tient’s comorbidities of chronic obstructive pulmonary disease on home oxygen, obstructive sleep apnoea
and morbid obesity. The pneumothorax was aspirated twice during the procedure, and required chest tube