Page 644 - Read Online
P. 644
John et al. Hepatoma Res 2020;6:56 I http://dx.doi.org/10.20517/2394-5079.2020.37 Page 3 of 9
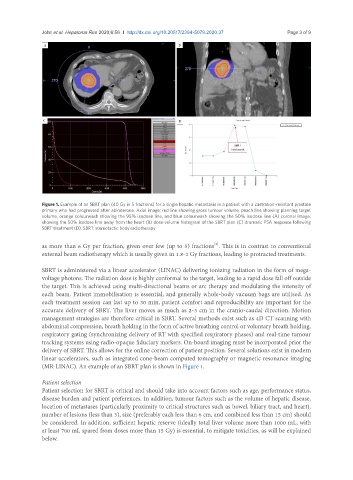
Figure 1. Example of an SBRT plan (40 Gy in 5 fractions) for a single hepatic metastasis in a patient with a castration-resistant prostate
primary who had progressed after abiraterone. Axial image; red line showing gross tumour volume, peach line showing planning target
volume, orange colourwash showing the 95% isodose line, and blue colourwash showing the 50% isodose line (A) coronal image;
showing the 50% isodose line away from the heart (B) dose-volume histogram of the SBRT plan (C) dramatic PSA response following
SBRT treatment (D). SBRT: stereotactic body radiotherapy
[6]
as more than 6 Gy per fraction, given over few (up to 5) fractions . This is in contrast to conventional
external beam radiotherapy which is usually given in 1.8-2 Gy fractions, leading to protracted treatments.
SBRT is administered via a linear accelerator (LINAC) delivering ionizing radiation in the form of mega-
voltage photons. The radiation dose is highly conformal to the target, leading to a rapid dose fall off outside
the target. This is achieved using multi-directional beams or arc therapy and modulating the intensity of
each beam. Patient immobilisation is essential, and generally whole-body vacuum bags are utilised. As
each treatment session can last up to 30 min, patient comfort and reproducibility are important for the
accurate delivery of SBRT. The liver moves as much as 2-3 cm in the cranio-caudal direction. Motion
management strategies are therefore critical in SBRT. Several methods exist such as 4D CT scanning with
abdominal compression, breath holding in the form of active breathing control or voluntary breath holding,
respiratory gating (synchronizing delivery of RT with specified respiratory phases) and real-time tumour
tracking systems using radio-opaque fiduciary markers. On-board imaging must be incorporated prior the
delivery of SBRT. This allows for the online correction of patient position. Several solutions exist in modern
linear accelerators, such as integrated cone-beam computed tomography or magnetic resonance imaging
(MR-LINAC). An example of an SBRT plan is shown in Figure 1.
Patient selection
Patient selection for SBRT is critical and should take into account factors such as age, performance status,
disease burden and patient preferences. In addition, tumour factors such as the volume of hepatic disease,
location of metastases (particularly proximity to critical structures such as bowel, biliary tract, and heart),
number of lesions (less than 3), size (preferably each less than 6 cm, and combined less than 15 cm) should
be considered. In addition, sufficient hepatic reserve (ideally total liver volume more than 1000 mL, with
at least 700 mL spared from doses more than 15 Gy) is essential, to mitigate toxicities, as will be explained
below.