Page 253 - Read Online
P. 253
Cao Cancer Evo-Dev
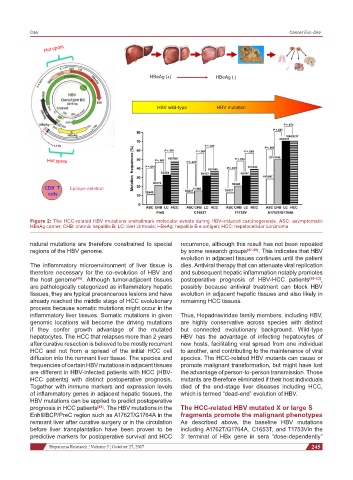
Hot spots
HBeAg (+) HBeAg (-)
HBV wild-type HBV mutation
Hot spots
+
CD8 T Epitope deletion
cells
Figure 2: The HCC-related HBV mutations arehallmark molecular events during HBV-induced carcinogenesis. ASC: asymptomatic
HBsAg carrier; CHB: chronic hepatitis B; LC: liver cirrhosis; HBeAg: hepatitis B e antigen; HCC: hepatocellular carcinoma
natural mutations are therefore constrained to special recurrence, although this result has not been repeated
regions of the HBV genome. by some research groups [47-49] . This indicates that HBV
evolution in adjacent tissues continues until the patient
The inflammatory microenvironment of liver tissue is dies. Antiviral therapy that can attenuate viral replication
therefore necessary for the co-evolution of HBV and and subsequent hepatic inflammation notably promotes
the host genome [45] . Although tumor-adjacent tissues postoperative prognosis of HBV-HCC patients [50-53] ,
are pathologically categorized as inflammatory hepatic possibly because antiviral treatment can block HBV
tissues, they are typical precancerous lesions and have evolution in adjacent hepatic tissues and also likely in
already reached the middle stage of HCC evolutionary remaining HCC tissues.
process because somatic mutations might occur in the
inflammatory liver tissues. Somatic mutations in given Thus, Hepadnaviridae family members, including HBV,
genomic locations will become the driving mutations are highly conservative across species with distinct
if they confer growth advantage of the mutated but connected evolutionary background. Wild-type
hepatocytes. The HCC that relapses more than 2 years HBV has the advantage of infecting hepatocytes of
after curative resection is believed to be mostly recurrent new hosts, facilitating viral spread from one individual
HCC and not from a spread of the initial HCC cell to another, and contributing to the maintenance of viral
diffusion into the remnant liver tissue. The species and species. The HCC-related HBV mutants can cause or
frequencies of certain HBV mutations in adjacent tissues promote malignant transformation, but might have lost
are different in HBV-infected patients with HCC (HBV- the advantage of person-to-person transmission. Those
HCC patients) with distinct postoperative prognosis. mutants are therefore eliminated if their host individuals
Together with immune markers and expression levels died of the end-stage liver diseases including HCC,
of inflammatory genes in adjacent hepatic tissues, the which is termed “dead-end” evolution of HBV.
HBV mutations can be applied to predict postoperative
prognosis in HCC patients [46] . The HBV mutations in the The HCC-related HBV mutated X or large S
EnhII/BCP/PreC region such as A1762T/G1764A in the fragments promote the malignant phenotypes
remnant liver after curative surgery or in the circulation As described above, the baseline HBV mutations
before liver transplantation have been proven to be including A1762T/G1764A, C1653T, and T1753Vin the
predictive markers for postoperative survival and HCC 3’ terminal of HBx gene in sera “dose-dependently”
Hepatoma Research ¦ Volume 3 ¦ October 27, 2017 245