Page 215 - Read Online
P. 215
Giakoustidis et al. Sorafenib-everolimus for metastases after liver-transplantation
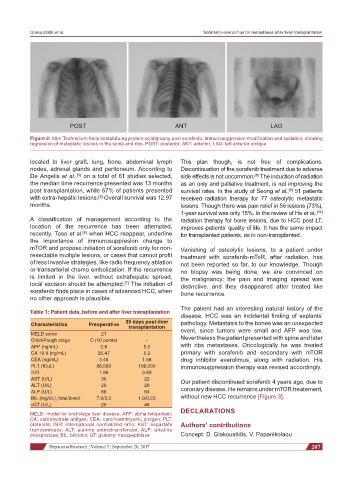
POST ANT LAO
Figure 2: 99m Technetium helix destabilizing protein scintigraphy post sorafenib, immunosuppresion modification and radiation, showing
regression of metastatic lesions in the spine and ribs. POST: posterior; ANT: anterior; LAO: left anterior oblique
located to liver graft, lung, bone, abdominal lymph This plan though, is not free of complications.
nodes, adrenal glands and peritoneum. According to Discontinuation of the sorafenib treatment due to adverse
De Angelis et al., on a total of 61 studies selected, side effects is not uncommon. The induction of radiation
[5]
[8]
the median time recurrence presented was 13 months as an only and palliative treatment, is not improving the
post transplantation, while 67% of patients presented survival rates. In the study of Seong et al., 51 patients
[9]
with extra-hepatic lesions. Overall survival was 12.97 received radiation therapy for 77 osteolytic metastatic
[5]
months. lesions. Though there was pain relief in 56 lesions (73%),
1-year survival was only 15%. In the review of He et al.,
[10]
A classification of management according to the radiation therapy for bone lesions, due to HCC post LT,
location of the recurrence has been attempted, improves patients’ quality of life. It has the same impact
recently. Toso et al. when HCC reappear, underline for transplanted patients, as in non-transplanted.
[6]
the importance of immunosuppresion change to
mTOR and propose initiation of sorafenib only for non- Vanishing of osteolytic lesions, to a patient under
resectable multiple lesions, or cases that cannot profit treatment with sorafenib-mToR, after radiation, has
of less invasive strategies, like radio frequency ablation not been reported so far, to our knowledge. Though
or transarterial chemo embolization. If the recurrence no biopsy was being done, we are convinced on
is limited in the liver, without extrahepatic spread, the malignancy: the pain and imaging spread was
local excision should be attempted. The initiation of distinctive, and they disappeared after treated like
[7]
sorafenib finds place in cases of advanced HCC, when bone recurrence.
no other approach is plausible.
The patient had an interesting natural history of the
Table 1: Patient data, before and after liver transplantation
disease. HCC was an incidental finding of explants’
30 days post-liver pathology. Metastasis to the bones was an unexpected
Characteristics Preoperative transplantation
MELD score 21 - event, since tumors were small and AFP was low.
Child-Pough stage C (10 points) - Nevertheless the patient presented with spine and later
AFP (ng/mL) 2.8 5.2 with ribs metastases. Oncologically he was treated
CA 19-9 (ng/mL) 25.47 5.2 primary with sorafenib and secondary with mTOR
CEA (ng/mL) 3.46 1.58 drug inhibitor everolimus, along with radiation. His
PLT (K/μL) 66,000 109,000 immunosuppression therapy was revised accordingly.
INR 1.96 0.89
AST (U/L) 36 22 Our patient discontinued sorafenib 4 years ago, due to
ALT (U/L) 20 29 coronary disease. He remains under mTOR treatement,
ALP (U/L) 88 64
BIL (mg/dL), total/direct 7.0/3.3 1.0/0.23 without new HCC recurrence [Figure 3].
γGT (U/L) 20 46
DECLARATIONS
MELD: model for end-stage liver disease; AFP: alpha fetoprotein;
CA: carbohydrate antigen; CEA: carcinoembryonic antigen; PLT:
platelets; INR: international normalized ratio; AST: aspartate Authors’ contributions
transaminase; ALT: alanine aminotransferase; ALP: alkaline
phosphatase; BIL: bilirubin; GT: glutamyl transpeptidase Concept: D. Giakoustidis, V. Papanikolaou
Hepatoma Research ¦ Volume 3 ¦ September 20, 2017 207