Page 108 - Read Online
P. 108
Diet history depicted no gastrointestinal (GI) symptoms, Eastern Cooperative Oncology Group (ECOG)
dental or oral problem, or food allergies. The simplified performance status score of 3 indicated that the
nutritional appetite questionnaire (SNAQ) score was patient was capable of only limited self-care and
16 hence there was no significant risk of at least unable to carry out any work activities that was ≥ 50%
[13]
5% weight loss within 6 months. The patient was of working hours. Quality of life (QOL) assessment
[11]
by short form-36 before LT depicted low level in its
[12]
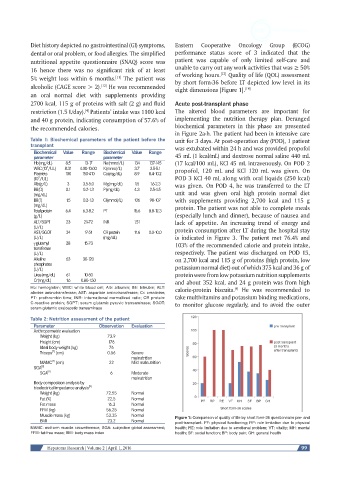
alcoholic (CAGE score > 2). He was recommended eight dimensions [Figure 1]. [14]
an oral normal diet with supplements providing
2700 kcal, 115 g of proteins with salt (2 g) and fluid Acute post-transplant phase
restriction (1.5 L/day). Patients’ intake was 1100 kcal The altered blood parameters are important for
[4]
and 40 g protein, indicating consumption of 57.6% of implementing the nutrition therapy plan. Deranged
the recommended calories. biochemical parameters in this phase are presented
in Figure 2a-h. The patient had been in intensive care
Table 1: Biochemical parameters of the patient before the unit for 3 days. At post-operation day (POD), 1 patient
transplant was extubated within 24 h and was provided propofol
Biochemical Value Range Biochemical Value Range
parameter parameter 45 mL (1 kcal/mL) and dextrose normal saline 440 mL
Hb (mg/dL) 8.5 13-17 Na (mmol/L) 134 137-145 (17 kcal/100 mL), KCl 45 mL intravenously. On POD 2
3
WBC (10 /UL) 8.31 4.00-10.00 K (mmol/L) 3.7 3.5-5.1 propofol, 120 mL and KCl 120 mL was given. On
Platelets 100 150-410 Ca (mg/dL) 8.9 8.4-10.2
3
(10 /UL) POD 3 KCl 40 mL along with oral liquids (250 kcal)
Alb (g/L) 3 3.5-5.0 Mg (mg/dL) 1.5 1.6-2.3 was given. On POD 4, he was transferred to the LT
Bili (D) 0.1 0.2-1.3 P (mg/dL) 4.3 2.5-4.5
(mg/dL) unit and was given oral high protein normal diet
Bili (T) 1.5 0.2-1.3 Cl (mmol/L) 106 98-107 with supplements providing 2,700 kcal and 115 g
(mg/dL) protein. The patient was not able to complete meals
Total protein 6.4 6.3-8.2 PT 15.6 8.8-12.3
(g/L) (especially lunch and dinner), because of nausea and
ALT/SGPT 23 21-72 INR 1.51 lack of appetite. An increasing trend of energy and
(U/L) protein consumption after LT during the hospital stay
AST/SGOT 34 17-51 CR protein 11.6 0.0-10.0
(U/L) (mg/dL) is indicated in Figure 3. The patient met 76.4% and
γ glutamyl 28 15-73 103% of the recommended calorie and protein intake,
transferase
(U/L) respectively. The patient was discharged on POD 15,
Alkaline 63 30-120 on 2,700 kcal and 115 g of proteins (high protein, low
phosphates
(U/L) potassium normal diet) out of which 375 kcal and 36 g of
Urea (mg/dL) 61 10-50 protein were from low potassium nutrition supplements
Cr (mg/dL) 1.6 0.80-1.50 and about 352 kcal, and 24 g protein was from high
Hb: hemoglobin; WBC: white blood cell; Alb: albumin; Bili: bilirubin; ALT: calorie-protein biscuits. He was recommended to
[4]
alanine aminotransferase; AST: aspartate aminotransferase; Cr: creatinine;
PT: prothrombin time; INR: international normalized ratio; CR protein: take multivitamins and potassium binding medications,
C-reactive protein; SGPT: serum glutamic pyruvic transaminase; SGOT: to monitor glucose regularly, and to avoid the outer
serum glutamic oxaloacetic transaminase
Table 2: Nutrition assessment of the patient
Parameter Observation Evaluation
Anthropometric evaluation
Weight (kg) 73.9
Height (cm) 176
Ideal body weight (kg) 76
[7]
Triceps (cm) 0.56 Severe
malnutrition
[7]
MAMC (cm) 22 Mild malnutrition
SGA [8]
SGA [8] 6 Moderate
malnutrition
Body composition analysis by
bioelectrical impedance analysis [9]
Weight (kg) 72.55 Normal
Fat (%) 22.5 Normal
Fat mass 16.3 Normal
FFM (kg) 56.25 Normal
Muscle mass (kg) 53.35 Normal Figure 1: Comparison of quality of life by short form-36 questionnaire pre- and
BMI 23.2 Normal post-transplant. PF: physical functioning; RP: role limitation due to physical
MAMC: mid-arm muscle circumference; SGA: subjective global assessment; health; RE: role limitation due to emotional problem; VT: vitality; MH: mental
FFM: fat-free mass; BMI: body mass index health; SF: social function; BP: body pain; GH: general health
Hepatoma Research | Volume 2 | April 1, 2016 99