Page 472 - Read Online
P. 472
Saadi et al. Vessel Plus 2020;4:41 I http://dx.doi.org/10.20517/2574-1209.2020.54 Page 11 of 14
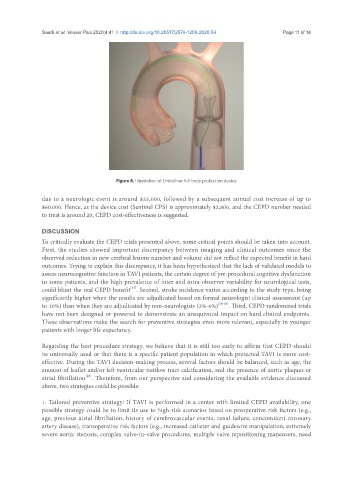
Figure 8. Illustration of Emboliner full body protection device
due to a neurologic event is around $25,000, followed by a subsequent annual cost increase of up to
$60.000. Hence, as the device cost (Sentinel CPS) is approximately $2,800, and the CEPD number needed
to treat is around 20, CEPD cost-effectiveness is suggested.
DISCUSSION
To critically evaluate the CEPD trials presented above, some critical points should be taken into account.
First, the studies showed important discrepancy between imaging and clinical outcomes since the
observed reduction in new cerebral lesions number and volume did not reflect the expected benefit in hard
outcomes. Trying to explain this discrepancy, it has been hypothesized that the lack of validated models to
assess neurocognitive function in TAVI patients, the certain degree of pre-procedural cognitive dysfunction
in some patients, and the high prevalence of inter and intra-observer variability for neurological tests,
[15]
could blunt the real CEPD benefit . Second, stroke incidence varies according to the study type, being
significantly higher when the results are adjudicated based on formal neurologist clinical assessment (up
to 10%) than when they are adjudicated by non-neurologists (2%-6%) [24-26] . Third, CEPD randomized trials
have not been designed or powered to demonstrate an unequivocal impact on hard clinical endpoints.
These observations make the search for preventive strategies even more relevant, especially in younger
patients with longer life expectancy.
Regarding the best procedure strategy, we believe that it is still too early to affirm that CEPD should
be universally used or that there is a specific patient population in which protected TAVI is more cost-
effective. During the TAVI decision-making process, several factors should be balanced, such as age, the
amount of leaflet and/or left ventricular outflow tract calcification, and the presence of aortic plaques or
[26]
atrial fibrillation . Therefore, from our perspective and considering the available evidence discussed
above, two strategies could be possible:
1. Tailored preventive strategy: If TAVI is performed in a center with limited CEPD availability, one
possible strategy could be to limit its use to high-risk scenarios based on preoperative risk factors (e.g.,
age, previous atrial fibrillation, history of cerebrovascular events, renal failure, concomitant coronary
artery disease), transoperative risk factors (e.g., increased catheter and guidewire manipulation, extremely
severe aortic stenosis, complex valve-in-valve procedures, multiple valve repositioning maneuvers, need